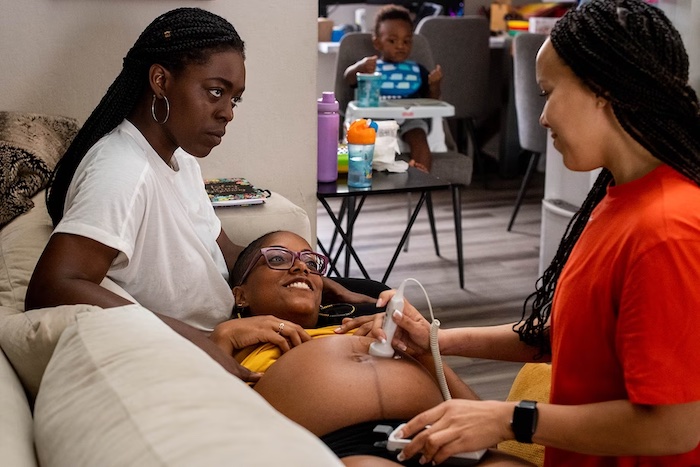
When sheriff’s deputies in Florida went to perform a welfare check last month on Tori Bowie, the Olympic runner, they made the saddest possible discovery. Bowie and her newborn daughter were dead. Though the full story of Bowie’s last days has yet to emerge, some details are clear: She had died in labor, suffering from eclampsia and respiratory distress.
These tragic events are an enraging reminder that the United States’ maternal mortality rate is the worst in the industrialized world. Black women are up to three times more likely to die during or after pregnancy than White women. Almost two-thirds of all these deaths could be prevented.
Expectant moms deserve more from their lawmakers, providers, public health groups and hospitals: more visits before and after pregnancy, better access to the simple drugs and devices that could keep them alive, and expanded insurance coverage.
Since the federal government began keeping records in 1987, America’s maternal mortality rate has only gotten worse. Between 2000 and 2020, the United States was one of eight countries where the situation deteriorated fastest, a list that included Venezuela and Mauritius. There’s no one cause of this long slide: A strained health-care system, a stingy insurance system, a lack of paid leave, the retreat of reproductive rights and endemic racism all contribute.
Covid-19 made a bad situation worse. Pregnant women who contracted the virus were seven times more likely to die than those who avoided infection. But even as vaccination became widespread, pregnant women kept dying from all the more common causes: infections, hemorrhages, hypertensive disorders such as preeclampsia and embolisms. In 2022, 733 American women died while pregnant or shortly after childbirth. That’s a maternal death rate of 20 per 100,000 births — up from 17.6 in 2019, already two or three times the rate of many high-income nations.
For Black women, pregnancy and childbirth bring the toll of racism in the United States into sharp focus. A large body of research shows that being Black in America wears on women’s bodies, leaving them uniquely vulnerable during pregnancy. Black women are 60 percent more likely than White women to experience preeclampsia, for instance. Add to which they experience inequalities in access, quality of care, prescribing, data collection and more. These differences persist even among wealthy, educated women. So stark is the disparity it has come under United Nations scrutiny.
There’s much providers can do to help: A 2019 analysis of preventable maternal deaths by the Centers for Disease Control and Prevention gives a clear list. Open earlier or stay open later to serve patients who work nights. Accept Medicaid. Educate patients early and often about conditions to watch out for. Take patients with headaches or shortness of breath seriously.
And there’s a lot policymakers must do to keep pregnant women safe and healthy. Fortunately, even in this divided, fractious Congress, there’s bipartisan support. Bills introduced by Reps. Lauren Underwood (D-Ill.), Robin L. Kelly (D-Ill.) and Robert E. Latta (R-Ohio) and Sens. Charles E. Grassley (R-Iowa) and Maggie Hassan Wood (D-N.H.) would pull together working groups to identify the best ways forward. One target of Kelly and Latta’s: Finding ways to identify and improve hospitals and doctors who are failing women and babies.
Lawmakers in both parties agree that childbirth and postpartum support from other practitioners matters, too. Evidence is accumulating that access to doula care during labor can lower Caesarean section rates. Doulas offer mothers nonmedical support and advocacy before, during and after delivery. Programs run both by community groups and insurance giants are exploring whether doulas can have a measurable impact on maternal mortality, especially for Black women.
Congress funded some home health visiting programs in the 2022 government appropriations bill. The United States should join other wealthy countries in making sure new mothers get regular visits after they come home from the hospital, when they are still at risk.
It would also help to standardize how Medicaid covers the medicines and devices for pregnant people. An analysis by KFF found glaring gaps. Four state Medicaid programs still don’t cover low-dose aspirin, which can prevent preeclampsia. Ten don’t cover blood pressure monitors for use at home between doctor’s visits. And six states don’t cover glucose monitors, crucial for managing gestational diabetes.
Meanwhile, the federal government could kick-start pilot programs that explore new ways to lower maternal mortality. Examples include payment schemes that compensate providers who do a better job for mothers and babies or demonstration projects that bundle housing and prenatal care in the same setting.
We don’t know whether Tori Bowie and her baby could have been saved with earlier intervention. We do know how to save hundreds of other American mothers.
Complete Article ↪HERE↩!
