By Netana Markovitz
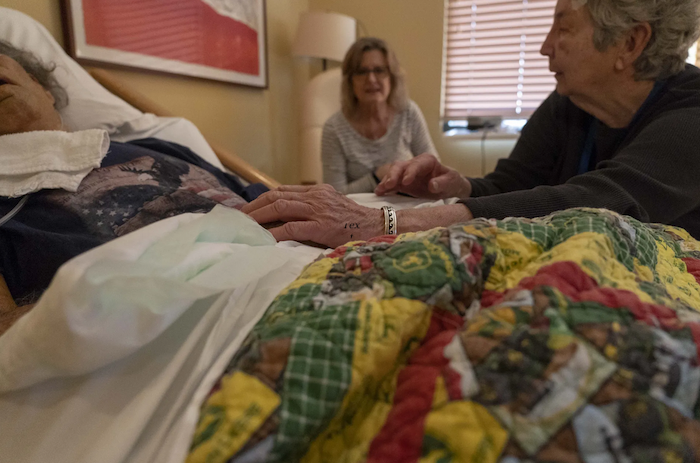
When Jordana Fremed, 26, got engaged, she didn’t think that one of the first serious topics the couple would discuss would be death and dying. But soon after, her fiance’s mother was diagnosed with amyotrophic lateral sclerosis, prompting difficult discussions to plan his mother’s end-of-life care.
Eventually, the couple started talking about wishes for their medical care should they be sick or injured and unable to communicate.
The experience “definitely got us thinking about those questions in relation to what we might want for ourselves,” said Fremed, of Teaneck, N.J.
Medical experts such as Rebecca Sudore, palliative medicine physician and geriatrician at the University of California at San Francisco, say that faced with these numbers, more young people should consider advance-care planning — a process that helps people think through medical decision-making should they be unable to communicate themselves.
“You know the old saying, ‘I could get hit by a bus tomorrow?’ And actually you could,” Sudore said. “And covid has shown us, too, that things are unpredictable. For people in their 20s or 30s who don’t have a serious illness, it could be helpful to think, ‘Well, if I did get hit by a bus tomorrow, who would speak up for me?’ ”
Sudore said she thinks that advance-care planning is an important way for people to participate in their own medical care. “People, particularly in their 20s, can think about advance-care planning as a way to prepare for medical decision-making and really to ensure that people have a voice in their health care, both now and in the future,” she said.
Advance-care planning is an umbrella term that may include completing advance directives — documents that provide written instructions for loved ones and a medical team. They may include specific instructions about which medical interventions doctors can perform — or withhold — such as CPR, mechanical ventilation or artificial nutrition.
Directives can also include broader descriptions of what a person considers a good quality of life, such as the ability to run or spend time with family.
These descriptions can help doctors imagine what a patient would want if they could communicate themselves and determine what medical interventions to offer.
Finally, advance directives often designate an individual to make medical decisions on a person’s behalf, should that person become incapacitated.
“It’s important for every person to think about this topic because unexpected and tragic things happen every day,” said Laura Taylor, a palliative care physician at the University of Michigan. “The pandemic has taught us is that even completely healthy adults can develop serious or life-threatening illness from covid-19, especially with the spread of more virulent variants like delta. And some of those people will require a surrogate decision-maker.”
While less likely to die than older adults, Americans in their 20s and 30s do face risks. The three leading causes of death in adults ages 25 to 34 in 2019 were unintentional injury, suicide and homicide, according to data from the Centers for Disease Control and Prevention. As of Jan. 19, over 5,000 adults between the ages of 18 and 29 in the United States have died of covid-19 since the start of the pandemic, according to provisional data from the CDC. Three hundred per 100,000 adults in this age group have been hospitalized.
In advance-care planning, young adults should first consider who they would want to make decisions on their behalf should they be unable to do so. That person is called a surrogate decision-maker or health-care proxy.
Experts agree that young, healthy adults should worry less about the nuances of medical decision-making, such as whether they would want to be intubated, and instead focus on designating a surrogate decision-maker.
“I think the majority of healthy young adults probably would default to receiving all aggressive, life-prolonging interventions that were offered to them if they were to become seriously ill, so it’s less important for young adults to have a detailed sense of their preferences and wishes,” Taylor said. “For young adults, it’s most important to identify the best surrogate decision-maker who understands that person well and can advocate for them.”
Legally, it might not be who they expect.
“People might assume ‘I want my roommate or my partner to make these decisions for me,’ ” Sudore said, “but it could be some estranged family member because that person is the next of kin.”
“I’m thinking about a young unmarried person who may not have a strong or trusted relationship with their parents, who may not want their parents to be their surrogate decision-makers, but they become their decision-makers by legal default,” Taylor said. “It’s really important for that person to decide who they would want to be assisting in medical decision-making for them if they were unable to.”
After choosing a surrogate, it is important to discuss health wishes together to ensure that the surrogate is comfortable making those decisions. Sudore recommended talking to the person about “what’s important in your life, and for your quality of life, and for your health care, so that this trusted person is really prepared to advocate for you if ever they needed to.”
Sudore is the founder and director of PREPARE for Your Care, an interactive site on advance-care planning. It yields a prepopulated advance directive for a specific location, as the process can vary by state. The documents can be updated at any point, should someone’s wishes or circumstances change.
“We have these easy-to-read advance directives,” Sudore said. “They focus on things like value, goals, what brings quality to somebody’s life, which is probably more important to someone in their 20s than ‘Do you want CPR or mechanical ventilation?’ ”
Olivia Duffield, 24, a medical student at Temple University in Philadelphia, first heard about advance-care planning during the terminal illness of a family member when she was a child. After learning more in a bioethics course, she broached the topic of her own wishes to her parents.
“For me, I think about what would happen if I were to get into a car accident or have a really sudden unexpected event that would cause me to potentially be brain dead or to be intubated in the hospital,” Duffield said.
Sudore said advance-care planning should be normalized for young people.
“When I think about it, it’s a kindness to ourselves in the sense that it gives us empowerment to make sure that our voice is heard if there’s a time that we could not speak for ourselves,” she said. “And it’s a kindness to our loved ones by giving them a little bit of a heads up.”
Fremed agrees: “You kind of always think that you have until tomorrow to do it, but things can happen in a moment. Having your other person know what your wishes are and what you want is just a very smart and healthy thing to do.”
Complete Article ↪HERE↩!