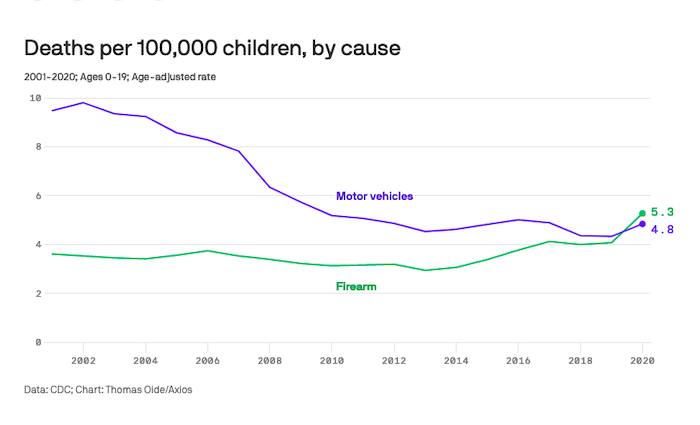
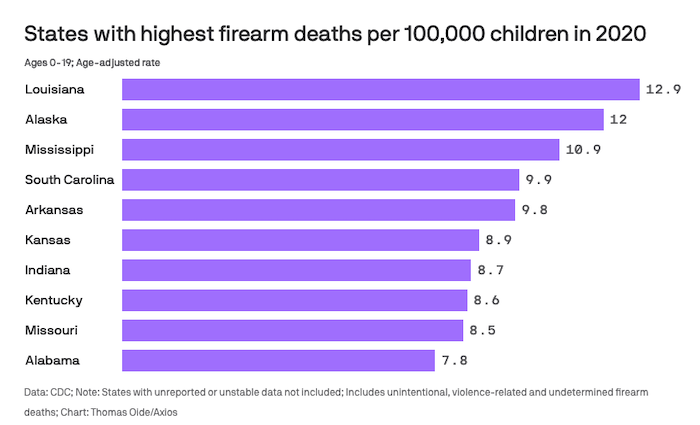
Voluntary assisted dying is now lawful in all Australian states. There is also widespread community support for it.
Yet some residential institutions, such as hospices and aged-care facilities, are obstructing access despite the law not specifying whether they have the legal right to do so.
As voluntary assisted dying is implemented across the country, institutions blocking access to it will likely become more of an issue.
So addressing this will help everyone – institutions, staff, families and, most importantly, people dying in institutions who wish to have control of their end.
The many ways to block access
While voluntary assisted dying legislation recognises the right of doctors to conscientiously object to it, the law is generally silent on the rights of institutions to do so.
While the institution where someone lives has no legislated role in voluntary assisted dying, it can refuse access in various ways, including:
- restricting staff responding to a discussion a resident initiates about voluntary assisted dying
- refusing access to health professionals to facilitate it, and
- requiring people who wish to pursue the option to leave the facility.
-
Here’s what happened to ‘Mary’
Here is a hypothetical example based on cases one of us (Charles Corke) has learned of via his role at Victoria’s Voluntary Assisted Dying Review Board.
We have chosen to combine several different cases into one, to respect the confidentiality of the individuals and organisations involved.
“Mary” was a 72-year-old widow who moved into a private aged-care facility when she could no longer manage independently in her own home due to advanced lung disease.
While her intellect remained intact, she accepted she had reached a stage at which she needed significant assistance. She appreciated the help she received. She liked the staff and they liked her.
After a year in the facility, during which time her lung disease got much worse, Mary decided she wanted access to voluntary assisted dying. Her children were supportive, particularly as this desire was consistent with Mary’s longstanding views.
Mary was open about her wish with the nursing home staff she felt were her friends.
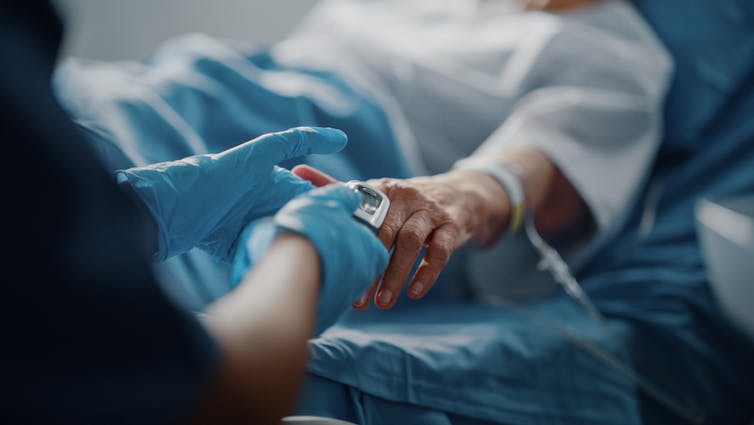
Mary’s condition worsened so she requested voluntary assisted dying. The executive management of the nursing home heard of her intentions. This resulted in a visit at which Mary was told, in no uncertain terms, her wish to access voluntary assisted dying would not be allowed. She would be required to move out, unless she agreed to change her mind.
Mary was upset. Her family was furious. She really didn’t want to move, but really wanted to continue with voluntary assisted dying “in her current home” (as she saw it).
Mary decided to continue with her wish. Her family took her to see two doctors registered to provide assessments for voluntary assisted dying, who didn’t work at the facility. Mary was deemed eligible and the permit was granted. Two pharmacists visited Mary at the nursing home, gave her the medication and instructed her how to mix it and take it.
These actions required no active participation from the nursing home or its staff.
Family and friends arranged to visit at the time Mary indicated she planned to take the medication. She died peacefully, on her own terms, as she wished. The family informed the nursing home staff their mother had died. Neither family nor staff mentioned voluntary assisted dying.
-
Staff are in a difficult position too
There is widespread community support for voluntary assisted dying. In a 2021 survey by National Seniors Australia, more than 85% of seniors agreed it should be available.
So it’s likely there will be staff who are supportive in most institutions. For instance, in a survey of attitudes to voluntary assisted dying in a large public tertiary hospital, 88% of staff supported it becoming lawful.
So a blanket policy to refuse dying patients access to voluntary assisted dying is likely to place staff in a difficult position. An institution risks creating a toxic workplace culture, in which clandestine communication and fear become entrenched.
-
What could we do better?
1. Institutions need to be up-front about their policies
Institutions need to be completely open about their policies on voluntary assisted dying and whether they would obstruct any such request in the future. This is so patients and families can factor this into deciding on an institution in the first place.
2. Institutions need to consult their stakeholders
Institutions should consult their stakeholders about their policy with a view to creating a “safe” environment for residents and staff – for those who want access to voluntary assisted dying or who wish to support it, and for those who don’t want it and find it confronting.
3. Laws need to change
Future legislation should define the extent of an institution’s right to obstruct a resident’s right to access voluntary assisted dying.
There should be safeguards in all states (as is already legislated in Queensland), including the ability for individuals to be referred in sufficient time to another institution, should they wish to access voluntary assisted dying.
Other states should consider whether it is reasonable to permit a resident, who does not wish to move, to be able to stay and proceed with their wish, without direct involvement of the institution.
Complete Article ↪HERE↩!