By Sarah Kaplan
The narrow, inscrutable zone between undeniably still here and unequivocally gone includes a range of states that look like life but may not be: a beating heart, a functioning digestive system, even moving fingers and toes. Death is less a moment then a process, a gradual drift out of existence as essential functions switch off, be it rapidly or one by one.
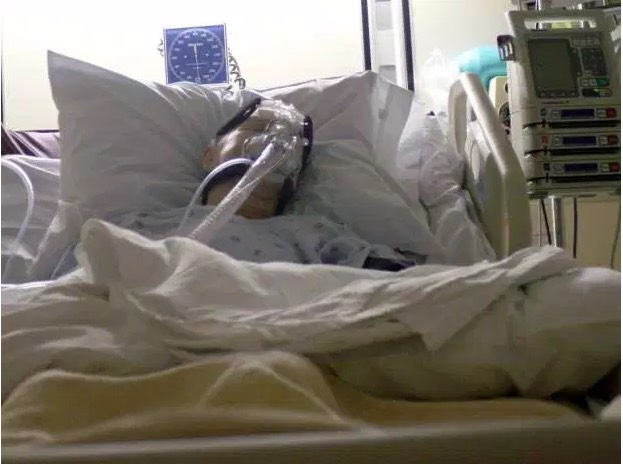
It was exactly midnight when Colleen Burns was wheeled into the operating room at St. Joseph’s Hospital Health Center in Syracuse, N.Y. She had been deep in a coma for several days after overdosing on a toxic cocktail of drugs. Scans of electrical activity in her brain were poor, and oxygen didn’t seem to be flowing. Burns was brain dead, her family was told; if they wanted to donate her organs, now was the time to do it.
But there, under the bright lights of the prep room in the OR, Burns opened her eyes. The 41-year-old wasn’t brain dead. She wasn’t even unconscious anymore. And doctors had been minutes away from cutting into her to remove her organs.
This is the nightmare scenario, the one that sends doctors and neurologists into cold sweats. It’s the reason that, in 2010, the American Academy of Neurology issued new guidelines for hospitals for determining brain death – the condition that legally demarcates life from whatever lies beyond. Those standards, according to Yale University neurologist David Greer, who worked on them, are meant to ensure that no patient is declared dead unless they really are beyond all hope of recovery.
“This is truly one of those matters of life and death, and we want to make sure this is done right every single time,” he told NPR.
But five years later, according to a study led by Greer that was published in the journal JAMA Neurology Monday, not all hospitals have adopted the guidelines.
Of the nearly 500 hospitals Greer and his colleagues surveyed over a three year period, most facilities did not require that someone with expertise in neurology or neurosurgery be present to determine brain death. At more than half of hospitals, the person who makes the call doesn’t even have to be the patient’s attending physician. A majority also didn’t require doctors to test for hypotension (abnormally low blood pressure) or hypothermia, both of which can suppress brain function which could mimic the appearance of brain death.
There were large improvements in standardization of brain death assessments across hospitals since the 2010 criteria were published. The survey also looked at standards, not practices.
But the lingering lapses are still worrying, Greer told NPR.
“There are very few things in medicine that should be black and white, but this is certainly one of them,” he said. “There really are no excuses at this point for hospitals not to be able to do this 100 percent of the time.”
Burns’s near-disastrous declaration of death happened in 2009, before the new guidelines were released, though a U.S. Department of Health and Human Services report on the incident found that St. Joseph’s had failed to meet previous standards for assessing death. Hospital staff missed several signs that Burns’s brain was still functioning the night she was due for organ donation surgery: her nostrils flared, her lips and tongue moved, she was breathing “above the ventilator” (meaning, taking breaths of her own accord). And when a nurse performed a reflex test, scraping a finger along the bottom of Burns’s foot, the woman’s toes curled inward, according to the Syracuse Post-Standard.
Doctors failed to order repeat CT scans and inexplicably and inaccurately said that she suffered from cardiac arrest when she hadn’t. Crucially, they also failed to measure whether the drugs she had taken still lingered in her system, preventing her from exhibiting even the most primitive reflexes expected of someone with brain activity.
This is a widespread problem, Greer’s report indicates: only about 32 percent of hospitals surveyed required drug tests to rule out toxic levels that can mimic the loss of primitive reflexes associated with brain death.
As soon as Burns opened her eyes, she was rushed back into the ICU and her doctors resumed treatment. She ultimately recovered from her overdose and was discharged two weeks later. But 16 months after the near-miss in the OR Burns committed suicide, her mother told the Post-Standard.
Burns’s mother, Lucille Kuss, said that depression, not what happened at the hospital, is what drove Burns to her death.
“She was so depressed that it really didn’t make any difference to her,” Kuss said of the incident.
Cases like Burns’s are increasingly rare, but they are emblematic of an anxiety at the root of all discussions about brain death. If death is a process, at what point in the process is the person no longer alive?
For most of history, this question was mostly moot. In the Victorian era, for example, doctors couldn’t keep blood pumping through a permanently unresponsive person’s body, even if they wanted to, and a person who lost brain function would surely quit breathing shortly after. Determining the exact point of death was less a medical necessity than a philosophical diversion: In the early 1900s, Boston doctor Duncan MacDougall recruited a number of terminally ill patients to lie down on a massive scale during their final moments. By measuring fluctuations in their weight at the moment they died, MacDougall claimed, he could determine the mass of the soul.
The advent of organ donation procedures in the 1960s changed that. That period of collapse as functions failed became not only a tragic inevitability, but a vital window when organs could be taken from a dead body and used to keep another alive. Yet defining that window is medically and ethically complicated. Open it too early, as Burns’s doctors almost did, and you risk sacrificing a patient who might have survived. Too late, and the organs will deteriorate along with the life they once sustained.
This is how we arrived at a definition of death as brain death, the complete and irreversible loss of brain function, including in the brain stem (which controls the heart and lungs). It comes largely from a 1968 definition written for the The Journal of the American Medical Association by an ad hoc Harvard Medical School committee, and then affirmed by a blue ribbon medical commission just over a decade later. A person can also be declared dead if they suffer an irreversible cessation of respiratory and circulatory functions – in other words, their heart and lungs permanently stop.
Some critics of brain death as a barometer for organ donation worry that it might encourage doctors to give up on their patients too soon.
Of course, the extraction of organs from a failing body is not the only reason to come up with a legal definition of death. It also helps hospitals to determine when and how to end life-saving interventions and remove a patient from life support.
The logic behind marking brain death as the end of life is that existence without a brain isn’t living.
“The brain is the person, the evolved person, not the machine person,” Cornell University neurologist Fred Plum said at a symposium on comas and death in 2000, according to the New Yorker. “. . . We are not one living cell. We are the evolution of a very large group of systems into the awareness of self and the environment.”
The brain is the person, the evolved person, not the machine person
But not everyone agrees. Cultural and legal definitions of life and death vary – in an interview with NPR, Georgetown University medical ethics professor Robert Veatch called defining death “the abortion question at the other end of life.”
Right now, the family of Jahi McMath, a California teenager who was declared brain dead two years ago but has been kept on life support, is suing to have her death certificate invalidated according to the Associated Press. The McMaths are devout Christians, their lawyer wrote in a brief, who believe that “as long as the heart is beating, Jahi is alive.”
McMath is currently on a ventilator in New Jersey, where state law allows hospitals to take a family’s religion into consideration when making decisions about end-of-life procedures.
Yet despite the legal, medical and moral complexities in determining brain death, there is no federally mandated procedure for doing so, according to the New York Times. There are only the guidelines issued by neurologists, and how hospitals choose to apply them.
That they do so inconsistently only exacerbates the anxieties people have about death and organ donation, Leslie Whetstine, a bioethicist at Walsh University in Ohio, told NPR.
“If one hospital is using a testing method that’s different from another hospital,” she said, “people might wonder: ‘Are they really dead?’”
Complete Article HERE!