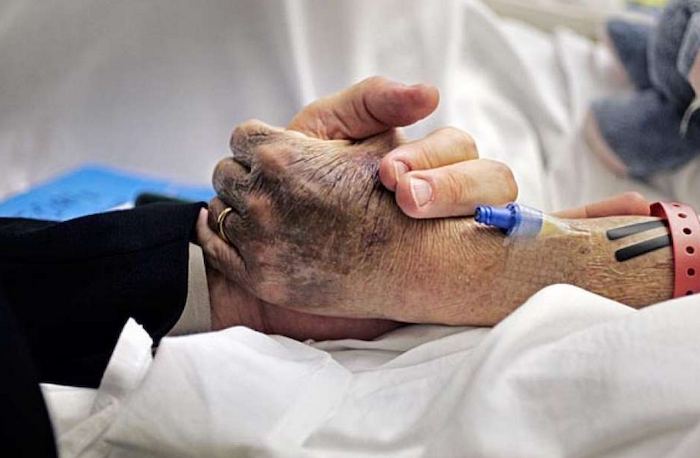
My parents lived good lives and expected to die good deaths. They exercised daily, ate plenty of fruits and vegetables, and kept, in their well-organized files, boilerplate advance health directives. But when he was 79, my beloved and seemingly vigorous father came up from his basement study, put on the kettle for tea, and had a devastating stroke. For the next 6½ years, my mother and I watched, heartbroken and largely helpless, as he descended into dementia, near-blindness and misery. To make matters worse, a pacemaker, thoughtlessly inserted two years after his stroke, unnecessarily prolonged his worst years on Earth.
That was a decade ago. Last month I turned 70. The peculiar problems of modern death — often overly medicalized and unnecessarily prolonged — are no longer abstractions to me. Even though I swim daily and take no medications, somewhere beyond the horizon, my death has saddled his horse and is heading my way. I want a better death than many of those I’ve recently seen.
In this I’m not alone. According to a 2017 Kaiser Foundation study, 7 in 10 Americans hope to die at home. But half die in nursing homes and hospitals, and more than a tenth are cruelly shuttled from one to the other in their final three days. Pain is a major barrier to a peaceful death, and nearly half of dying Americans suffer from uncontrolled pain. Nobody I know hopes to die in the soulless confines of an Intensive Care Unit. But more than a quarter of Medicare members cycle through one in their final month, and a fifth of Americans die in an ICU.
This state of affairs has many causes, among them fear, a culture-wide denial of death, ignorance of medicine’s limits, and a language barrier between medical staff and ordinary people. “They often feel abandoned at their greatest hour of need,” an HMO nurse told me about her many terminally ill patients. “But the oncologists tell us that their patients fire them if they are truthful.”
I don’t want this to be my story.
In the past three years, I’ve interviewed hundreds of people who have witnessed good deaths and hard ones, and I consulted top experts in end-of-life medicine. This is what I learned about how to get the best from our imperfect health care system and how to prepare for a good end of life.
Have a vision. Imagine what it would take you to die in peace and work back from there. Whom do you need to thank or forgive? Do you want to have someone reading to you from poetry or the Bible, or massaging your hands with oil, or simply holding them in silence? Talk about this with people you love.
Once you’ve got the basics clear, expand your horizons. A former forester, suffering from multiple sclerosis, was gurneyed into the woods in Washington state by volunteer firefighters for a last glimpse of his beloved trees. Something like this is possible if you face death while still enjoying life. Appoint someone with people skills and a backbone to speak for you if you can no longer speak for yourself.
Stay in charge. If your doctor isn’t curious about what matters to you or won’t tell you what’s going on in plain English, fire that doctor. That’s what Amy Berman did when a prominent oncologist told her to undergo chemotherapy, a mastectomy, radiation and then more chemo to treat her stage-four inflammatory breast cancer.
She settled on another oncologist who asked her, “What do you want to accomplish?” Berman said that she was aiming for a “Niagara Falls trajectory:” To live as well as possible for as long as possible, followed by a rapid final decline.
Berman, now 59, went on an estrogen suppressing pill. Eight years, later, she’s still working, she’s climbed the Great Wall of China, and has never been hospitalized. “Most doctors,” she says, “focus only on length of life. That’s not my only metric.”
Know the trajectory of your illness. If you face a frightening diagnosis, ask your doctor to draw a sketch tracking how you might feel and function during your illness and its treatments. A visual will yield far more helpful information than asking exactly how much time you have left.
When you become fragile, consider shifting your emphasis from cure to comfort and find an alternative to the emergency room.
And don’t be afraid to explore hospice sooner rather than later. It won’t make you die sooner, it’s covered by insurance, and you are more likely to die well, with your family supported and your pain under control.
Find your tribe and arrange caregivers. Dying at home is labor-intensive. Hospices provide home visits from nurses and other professionals, but your friends, relatives and hired aides will be the ones who empty bedpans and provide hands-on care. You don’t have to be rich, or a saint, to handle this well. You do need one fiercely committed person to act as a central tent pole and as many part-timers as you can marshal. People who die comfortable, well-supported deaths at home tend to have one of three things going for them: money, a rich social network of neighbors or friends, or a good government program (like PACE, the federal Program of All Inclusive Care for the Elderly).
Don’t wait until you’re at death’s door to explore your passions, deepen your relationships and find your posse. Do favors for your neighbors and mentor younger people. It doesn’t matter if you find your allies among fellow quilters, bridge-players, tai chi practitioners, or in the Christian Motorcyclists Association. You just need to share an activity face-to-face.
Take command of the space. No matter where death occurs, you can bring calm and meaning to the room. Don’t be afraid to rearrange the physical environment. Weddings have been held in ICUs so that a dying mother could witness the ceremony. In a hospital or nursing home, ask for a private room, get televisions and telemetry turned off, and stop the taking of vital signs.
Clean house: Hospice nurses often list five emotional tasks for the end of life: thank you, I love you, please forgive me, I forgive you, and goodbye. Do not underestimate the power of your emotional legacy, expressed in even a small, last-minute exchange. Kathy Duby of Mill Valley was raised on the East Coast by a violent alcoholic mother. She had no memory of ever hearing, “I love you.”
When Duby was in her 40s, her mother lay dying of breast cancer in a hospital in Boston. Over the phone, she told Duby, “Don’t come, I don’t want to see you.” Duby got on a plane anyway.
She walked into the hospital room to see a tiny figure curled up in bed — shrunken, yellow, bald, bronzed by jaundice, as Duby later wrote in a poem. Duby’s mother said aloud, “I love you and I’m sorry.”
Duby replied, “I love you and I’m sorry.”
“Those few moments,” Duby said, “Cleared up a lifetime of misunderstanding each other.”
Think of death as a rite of passage. In the days before effective medicine, our ancestors were guided by books and customs that framed dying as a spiritual ordeal rather than a medical event. Without abandoning the best of what modern medicine has to offer, return to that spirit.
Over the years, I’ve learned one thing: Those who contemplate their aging, vulnerability and mortality often live better lives and experience better deaths than those who don’t. They enroll in hospice earlier, and often feel and function better — and sometimes even live longer — than those who pursue maximum treatment.
We influence our lives, but we don’t control them, and the same goes for how they end. No matter how bravely you adapt to loss and how cannily you navigate our fragmented health system, dying will still represent the ultimate loss of control.
But you don’t have to be a passive victim. You retain moral agency. You can keep shaping your life all the way to its end — as long as you seize the power to imagine, to arrange support and to plan.
Complete Article ↪HERE↩!

















 “It was January in Seattle,” Anne said. “The sun was coming through the window and we could hear the market below beginning to wake up. We were just the three of us, talking and sharing our stories about him and the things we loved and didn’t love, the things that had pissed us off but now we laughed about. I can’t ever, in words, express the sweetness of that moment.
“It was January in Seattle,” Anne said. “The sun was coming through the window and we could hear the market below beginning to wake up. We were just the three of us, talking and sharing our stories about him and the things we loved and didn’t love, the things that had pissed us off but now we laughed about. I can’t ever, in words, express the sweetness of that moment.
