A Tim Boon Poem

Tim Boon, RN is the CEO of Good Shepherd Community Care in Newton, MA. Share this poem with ALL the loved ones.

The Amateur's Guide To Death & Dying
Enhancing Life Near Death

Tim Boon, RN is the CEO of Good Shepherd Community Care in Newton, MA. Share this poem with ALL the loved ones.
By Bianca Nogrady
We can talk about good deaths and bad deaths, cheating death or embracing it, but the one thing that we all seem to reach for is this: when we die, we want to do it our way.
Tony Smith* says his mother and father were lucky, if such a word can be used for death.
For while they both experienced long-running, debilitating, and often traumatic health problems in the years before each of them died, when the time came, they died the way they wanted to.
Mr Smith’s father died suddenly in bed from a massive heart attack. His mother chose to be kept comfortable in her final days and hours, no heroic measures undertaken to prolong her life, no resuscitation to bring her back from the brink. She was surrounded by her family as she exited this world at age 78, which was, as Tony says, “on her terms”.
Asking someone how they want to die is awkwardly similar to the stock line from a Bond villain. But at a certain point in our lives, it is one of the most important questions for an individual to ask themselves, for a doctor to ask their patient, and for a family to ask their ailing loved one.
This question can make the difference between someone seeing out their final hours in a peaceful setting — at home, or in a hospice, or in a care facility — surrounded by loved ones, with the only medical interventions being ones to ease discomfort; or dying in a loud, busy, bright emergency department.
According to one of many surveys with similar results, a South Australian study found 70 per cent of people said they would want to die at home if they had a terminal illness and 19 per cent said a hospital.
But data from the Australian Institute of Health and Welfare showed that in 2011 about 35 per cent of older people died in an emergency care setting and just 3 per cent died in community care.
Dying in a hospital setting is also expensive; it accounts for nearly half of the health costs associated with dying in this group. According to a 2014 report from The Grattan Institute, each year more than $2 billion is spent on older people dying in hospital.
“About a third of all people who die in hospital have only one admission — the one in which they die,” the report’s authors wrote. “The average cost of that admission for those aged 50 and over is about $19,000.”
While some of us may want the full suite of medical options in our final days and hours, some of us want to avoid it at all costs. The thing we often forget is that we do have a choice.
Liz Callaghan, the chief executive of Palliative Care Australia, points out that while we go through an often exhaustive process of preparing for birth — going to classes, talking to our family, making a birth plan — when it comes to death there is little planning and very little conversation.
“We’re ignoring those conversations, and by ignoring them we’re leaving family and loved ones with no plan and no idea what we want at a very emotional and difficult time,” Ms Callaghan says.
The analogy with birth is a useful one because many of the same questions need to be considered:
But there is another very important question to be considered for those facing the end of their life, and one that is less likely to apply to a birthing situation: who should speak for you when you cannot?
This is where advance care plans and enduring guardianships become vitally important.
These documents are intended to inform family, friends and medical professionals of your wishes about the sort of medical care and interventions you want at the end of your life, and to authorise certain individuals to speak on your behalf and ensure those wishes are respected.
Their form varies somewhat across states and territories, but one constant is that they are legally binding. A doctor aware of an advance care directive but who acts against its instructions could face charges of assault.
Advance care plans ask a specific series of questions intended to make us think about what interventions we would want and under what conditions.
These documents can and do evolve over time: what we might want when we are still reasonably independent and of sound mind may be very different from what we might want when illness has narrowed our options and the few choices remaining may be intensive and largely futile.
For example, the NSW advance care plan for individuals in residential care asks questions such as “If my heart or breathing stops due to old age or irreversible (not curable) health problems my choice, if CPR is a treatment option, would be to a) please try to restart my heart or breathing (Attempt CPR), b) Please allow me to die a natural death. Do not try to restart my heart or breathing (NO CPR), or c) I cannot answer this question. Let my doctor decide.”
It also asks individuals to think about how acceptable, difficult, or unbearable their life would be if, for example, they couldn’t recognise family or loved ones; have to be fed through a tube in their stomach; or cannot talk, read or write.
It provides space for individuals to write about their specific request with respect to medical care and in particular, life-prolonging treatments they do not want to have.
Mr Smith’s mother had had these conversations with her family, and was very clear about her wishes.
“Mum had strict DNR [do not resuscitate] instructions, she didn’t want any kind of life support, she didn’t want unnatural prolonging of her life,” he says. “Even when she stopped eating near the end she wasn’t force-fed or anything.”
But Ms Callaghan says the true benefit of advance care plans lies not in the pieces of paper but in the conversations associated with them.
“If you have those conversations and discussions with your next of kin, they will be confident that whatever they decide on your behalf is what you want,” she says.
It’s no coincidence that an online initiative to provide families with a framework for a discussion around end-of-life choices is called The Conversation Project.
As a GP of 30 years in the Western Australian town of Mandurah, Frank Jones has had that conversation many, many times with his patients. It’s not always comfortable, but he knows how important it is.
“People don’t like talking about their own mortality,” says Dr Jones, also president of the Royal Australian College of General Practitioners. “But I think it’s really important as people do age that we initiate this conversation.”
While we might be a death-defying society on the whole, Dr Jones finds that the vast majority of individuals who have life-limiting illnesses with little hope of meaningful recovery are very happy to have the conversation with their doctor, and happy to work through the one-page explainer he gives them.
The bigger hurdle comes when he suggests they also discuss it with their families.
As effective as an advance care directive might be in getting individuals to decide how they would prefer to die, it’s useless unless it is shared and at least acknowledged by that individual’s loved ones; the people who will be responsible for acting on those wishes.
An advance care directive is also useless if the medical staff working with that individual don’t know about it.
Unfortunately, advance care directives are often missed in the panic and chaos that happens when someone with a chronic life-limiting illness is taken to hospital.
“In the middle of the night, if that elderly person has a fall, and is whisked off by ambulance to the hospital, the hospital has no idea, unless the family’s involved and unless they know there’s an advance health directive in place,” Dr Jones says.
Unless a person is actually carrying the advance directive with them when they go to hospital, or someone at that hospital knows their wishes, there’s every chance that health care professionals will do what they’re best at — try to save a life by any means possible.
This is why enduring guardianships are almost as important as advance care plans, because they identify the person or people who are legally authorised to speak on your behalf and communicate your wishes.
Those documents may need to be produced to establish that right in a situation where difficult decisions are being made, but they are an important part of ensuring that someone’s end-of-life choices are heard and acted on.
The other challenge for our health system and society is setting up the infrastructure needed to fully support people’s end-of-life choices, particularly if that choice involves dying at home.
Dr Hal Swerissen, co-author of the ‘Dying Well‘ report from the Grattan Institute, says Australia needs a competent, home-based palliative care system that can support and take the pressure off carers.
“It is a challenge but there are now some really good home-based palliative care services, such as Silver Chain,” Dr Swerissen says.
“They take all the referrals for palliative care in Perth — so they do a lot of deaths each year — and they get 60 per cent of people [referred to them] dying at home.”
As well as enabling so many to see out their final weeks and months of life at home, services such as Silver Chain could also prove to be cost-neutral to the health system.
Dr Swerissen and co-author Stephen Duckett estimated that home-based care for the last three months of life would cost an average of $6,000 per person. If 30 per cent of all deaths were to occur at home, this would amount to an extra $237 million cost to the health care system.
But if these individuals are dying at home, they are avoiding hospital and residential care facilities, which Dr Swerissen and Dr Duckett calculated as a potential $233 million cost saving.
Mr Smith’s mother had hoped to die at home, but the level of medical care she needed at the end of her life meant she spent her final weeks in a palliative care facility. It wasn’t her first choice, but Mr Smith says the level of care she and the family received was excellent.
“We took turns, my siblings and I, to stay all night with her. As much as she wasn’t at home, we were there.”
* Tony Smith has asked that his name be changed.
Complete Article ↪HERE↩!
By Judson Haims
While I enjoy almost every day of my job, I am often faced with formidable challenges. One of the most difficult challenges I encounter is discussing plans for end of life with family members, clients and my contemporaries.
During the course of life, most people are required to handle many stressful situations. One of the most stressful and life altering is dealing with the passing of a loved one. Even when families have had the forethought to discuss a shared plan and how to honor and execute the loved one’s wishes, managing emotions, fears and anxieties of family and friends can be tenuous.
When a loved one’s life nears its end, so many areas need to be addressed. Often, it is easy to become overwhelmed and, thus, become immobilized. However, for those who have chosen to accept that the end will eventually come and have taken the time to develop a thoughtful plan, much emotional pain can be spared.
Some of the specific topics that need to be addressed in developing a plan include:
“It is obviously one thing to write about what you should do to initiate these difficult, but necessary, discussions. However, it is quite another issue to face the reality of what to actually say when you are facing a loved one and thinking about how best to break the ice with the topic of death and dying.”
For those who have not yet had to experience end-of-life discussions and planning, you will eventually. Don’t shy away from the hard discussions.
It is important to make time and find a place to begin discussions revolving around end-of-life issues. Maybe a group situation might make it easier, such as during a time when families gather together. These conversations can benefit from the “safety in numbers” theory and tend to be more philosophical than one-to-one situations.
Generally speaking, there are four steps to expressing end-of-life wishes:
1. Ask the right question.
2. Record those answers.
3. Discuss among the pertinent people (i.e., family members, loved ones, doctors, attorneys, etc.).
4. File documents. Make certain the important documents are filed on your computer, given to medical providers, family and anyone else who may be involved in advocating.
For those who would like to learn about which documents should be in place when planning for end of life, here are some to consider: advanced directives, living wills, medical durable power of attorney and do not resuscitate orders. Here in Colorado, the Colorado Advance Directives Consortium has made available a document called the Medical Orders for Scope of Treatment, which is designed to help you convey what your wishes are for medical care at the end of your life.
It is obviously one thing to write about what you should do to initiate these difficult, but necessary, discussions. However, it is quite another issue to face the reality of what to actually say when you are facing a loved one and thinking about how best to break the ice with the topic of death and dying.
Should you choose to further educate yourself, there are a number of resources available to assist in starting a conversation: Conversation Starter Kit (the conversationproject.org), Aging with Dignity (www.agingwith dignity.org) and Take Charge of your Life (www.takechargeofyour life.org) are just a few that you may want to look into.
When end-of-life discussions take place among doctors, family and patients, all the participants tend to feel better. Medical treatment is usually handled with more professionalism and is more effective. And, perhaps the most difficult to measure, the stress of such a difficult situation is drastically reduced.
Complete Article ↪HERE↩!
By Sarah Simons
[S]hould doctors do everything they can to preserve life, or should some medical techniques, such as cardio-pulmonary resuscitation (CPR), be a matter of patient choice? Doctor Sarah Simons wades into the debate and argues that ‘do not resuscitate’ decisions are all about patients’ human rights.
Of all our human rights, the right to life is the one most often held up as the flagship, fundamental right: after all, without life, how can one learn, love, communicate, play or have a family?
The right to life is closely linked to the right to health. Under the International Covenant on Economic, Social and Cultural Rights, which the UK has signed and ratified, states are required to “recognise the right of everyone to the enjoyment of the highest attainable standard of physical and mental health”.
Protecting patients’ rights to life and health involves providing necessary life-saving treatment (known as resuscitation) if their life is threatened by serious illness or injury. It also involves enabling patients to live as well as possible for as long as possible: for example, by treating preventable diseases and encouraging people to adopt a healthy lifestyle. However, although many aspects of medicine and health are unpredictable, death is the one certainty for all of us.
In recent years, there has been much debate surrounding how healthcare practitioners should approach end-of-life issues with patients. A ‘good, natural death’ is increasingly recognised as a part of someone’s human right to life.
When healthcare professionals acknowledge that someone is approaching the final stages of their life, and no longer responding to life-saving treatment, treatment is not withdrawn, but instead, the goal is changed to treatment focussed on preserving the patient’s quality of life and managing their symptoms in accordance with their wishes. It’s important to draw a distinction between this and the ethical debate on euthanasia, which is altogether different from end-of-life care and natural death.
A ‘good, natural death’ is increasingly recognised as a part of someone’s human right to life.
This change of focus often includes completing a ‘Do Not Resuscitate’ (DNR) order, instructing healthcare teams not to carry out cardiopulmonary resuscitation (CPR) when the patients’ heart and lungs cease to work. This decision is usually made on the grounds of pre-existing medical conditions and poor physiological reserve and frailty, which mean that CPR will not be successful. A DNR should always take into account the patient’s informed opinion on the matter, or at least their next of kin’s.
A DNR decision only refers to CPR. The patient can still receive treatment for related issues, such as antibiotics for an infection, and all other life-preserving or life-saving treatments can be given until the patient’s heart and lungs stop working. A DNR decision never means that life-saving treatment is not given – the purpose of a DNR is to allow the patient to pass away naturally and peacefully, with dignity and without traumatic medical intervention.
Understanding the reality of CPR is vital to understanding why it is a human rights issue. CPR is used when someone has a cardiac arrest, which means they have suddenly stopped breathing and their heart has stopped beating.
CPR specifically refers to the chest compressions, electric shocks and artificial breathing technique used to stimulate and replicate the beating of the heart to pump blood around the body and the breaths taken to inflate the lungs with oxygen. This is effective when a sudden cardiac arrest occurs and someone’s organs stop unexpectedly, but the underlying mechanism of a cardiac arrest is very different from when the heart stops beating as part of the body’s natural decline at the end of life.
CPR is traumatic, undignified and usually unsuccessful in patients of all ages.
Sadly, despite Hollywood’s optimistic depictions of resuscitation, the reality is that CPR is often traumatic, undignified and usually unsuccessful in patients of all ages. CPR will not reverse years of gradually shrinking muscle mass, rejuvenate brains worn down by the steady decline of dementia, remove cancerous tumours or clear obstructed lungs weathered by years of COPD, which are often the underlying causes when someone’s heart and lungs have stopped.
CPR will cause bruising, vomiting, bleeding and broken ribs. CPR will render someone’s dying moments traumatic and undignified, and it will leave their friends and families with lasting memories of a failed, brutal resuscitation rather than a mental image of their loved one peacefully slipping away pain-free and asleep.
Guidance published by the General Medical Council (GMC) in 2016 emphasised the importance of recognising patients’ human rights in relation to decisions about CPR and end-of-life care. The guidance recognised that “provisions particularly relevant to decisions about attempting CPR include the right to life (Article 2) [and] the right to be free from inhuman or degrading treatment (Article 3)”.
Article 3 of the Human Rights Convention specifically refers to the right to protection from inhuman or degrading treatment, and understanding the brutal, traumatic reality of CPR is a crucial consideration when thinking about DNR decisions. The GMC goes on to reference “the right to respect for privacy and family life (Article 8), the right to freedom of expression, which includes the right to hold opinions and to receive information (Article 10) and the right to be free from discrimination in respect of these rights (Article 14).”
The GMC guidance also highlights that the Human Rights Act, (which incorporates the Human Rights Convention into UK law), “aims to promote human dignity and transparent decision-making”, which should also be key concerns for doctors making decisions across all aspects of medicine.
Having open, frank discussions about CPR, and end-of-life decisions in general, enables healthcare professionals and patients to make informed decisions together. Doing so empowers patients to ask questions and insist that their rights are respected. It gives patients time to talk to their loved ones about what’s important to them, including any religious considerations, before their health deteriorates to a point where these conversations may not be possible.
Having open, frank discussions about CPR … enables healthcare professionals and patients to make informed decisions together.
Avoiding these conversations, while perhaps understandable given that no-one likes to think of their loved ones dying, means that important questions may not get asked and the patient’s wishes may go unheard. Making decisions on CPR and other practical matters is important, but so is acknowledging that someone wants to spend their last days eating mint chocolate chip ice cream at home listening to a specific Eva Cassidy album whilst surrounded by their pets and children.
As the NHS turns 70 later this year, and continues to navigate the challenges of an ageing population, conversations about end-of-life care are more important than ever before. Grief and bereavement are difficult, emotionally charged topics of conversation, but death is a normal human process. Taking the opportunity to talk about what we want at the end of our lives empowers us to make informed decisions and ultimately help all of us to die well one day.
Complete Article ↪HERE↩!

A Medical Power of Attorney is a legal instrument that allows you to select the person that you want to make healthcare decisions for you if and when you become unable to make them for yourself. The person you pick is representative for purposes of healthcare decision-making.
Any kind of decision that is related to your health that you allow. You could limit your representative to certain types of decisions. (For example, the decision to put you on life support when there is no hope of you getting better.) On the other hand, you could allow your representative to make any healthcare decision that might come up. This includes decisions to give, withhold or withdraw informed consent to any type of health care, including but not limited to, medical and surgical treatments. Other decisions that may be included are psychiatric treatment, nursing care, hospitalization, treatment in a nursing home, home health care and organ donation.
A Living Will is a statement of decisions you made yourself. It tells the doctor that you do not want to be kept alive by machines, if there is no hope of getting better. A Medical Power of Attorney gives someone else the authority to make medical decisions for you if you are unable to make them for yourself. It is meant to deal with situations that you cannot predict. Because you cannot predict these situations, you cannot decide in advance what choice you would make. The Medical Power of Attorney allows you to pick the person that you trust to make to these kinds of decisions when you cannot make them yourself.
Yes. Any decisions that you make in your Living Will must be followed by the person you name as your Medical Power of Attorney.
A Medical Power of Attorney is used when you become unable to make healthcare decisions for yourself. For example, if you are unconscious after a car accident and you need a blood transfusion; if you are under anesthesia and you need to have a more extensive procedure than you initially consented to; or if you become mentally incompetent as a result of Alzheimer’s Disease and you need medical treatment.
A doctor or psychologist or advance practice nurse working with a doctor will make this determination. Commonly, the doctor will say that you lack the capacity to make healthcare decisions. He or she may also say that you are incapacitated. If you are conscious, you will be told that you have been found to be incapacitated and that your Medical Power of Attorney Representative will be making decisions regarding your treatment.
The doctor, psychologist or advance nurse practitioner will evaluate your ability to:
If the doctor determines that you are unable to do these things, they must write this in your medical records. The doctor’s statement must include the reason why you were found to lack capacity.
No. Simply being old or having a mental illness is not enough to support a finding that you do not have the capacity to make medical decisions. The doctor must complete the three part evaluation discussed above before he or she determines that you do not have the capacity to make healthcare decisions.
No. The person you name as your Medical Power of Attorney has no authority until you become unable to make your own decisions.
Yes. You may name one or more “successor representatives” to fill this role if your first choice is unable, unwilling or disqualified to serve.
The person that you name as your Medical Power of Attorney representative can make any decisions related to your health care that you allow. These decisions could include giving, withholding or withdrawing informed consent to any type of health care, including but not limited to, medical and surgical treatments. Other decisions that may be included are life-prolonging interventions, psychiatric treatment, nursing care, hospitalization, treatment in a nursing home, home health care and organ donation. Your representative can have or control access to your medical records and decide about measures for the relief of pain.
Your Medical Power of Attorney can be as broad or as narrow as you want it to be. You can specifically write that your Medical Power Attorney Representative shall not have the power to make one of these decisions. Or, you can specifically state exactly what decision you want your Medical Power of Attorney Representative to make. For example, you might say that your representative cannot give a certain person access to your medical records.
There are several things that you can do to help your representative make decisions that you would agree with.
You should pick someone that knows you well and that you trust to make healthcare decisions for you based on your personal wishes and values. You may or may not want to name a family member as your Medical Power of Attorney Representative. Keep in mind, that some of the decisions your representative will have to make will be very difficult. It might be difficult for some family members to overcome their own emotions and make decisions that are based on your personal values. The most important consideration in naming a Medical Power of Attorney Representative is to choose someone you trust to be able to make decisions based on the values and directions you have set out.
No, the law says that you cannot appoint your doctor as your Medical Power of Attorney. Additionally, the following people cannot serve as your Medical Power of Attorney:
No. A Medical Power of Attorney only gives the person you appoint authority to make healthcare related decisions. This does not include authority to pay your bills. For that you need a Durable Financial Power of Attorney. It is entirely possible that the same person may hold both your Medical Power of Attorney and your Financial Power of Attorney. However, if this is not the case, your Medical Power of Attorney Representative has no financial authority.
If you appoint a medical power of attorney and then someone petitions to have a guardian appointed for you, the court will give the person you appointed as medical power of attorney special consideration. In other words, the court will appoint the person you name as a medical power of attorney to be your guardian unless it finds that there is a good reason not to.
Yes. As long as you have the capacity to do so, you can revoke your Medical Power of Attorney at any time by any of these methods.
Yes, if you named your spouse as your Medical Power of Attorney Representative or successor representative. When a final divorce decree is granted, the appointment of your spouse is automatically revoked. You will need to sign a new power of attorney. If you still want your former spouse to serve as your representative, he or she may do so, provided that you reappoint the m in a new Medical Power of Attorney.
There are seven requirements:
This Medical Power of Attorney shall become effective only upon my incapacity to give, withdraw, or withhold informed consent to my own medical care.
*Persons under 18 are presumed to lack capacity. In order to defeat this presumption, persons under 18 must undergo an examination by a doctor, or psychologist, or an advance practice nurse who is collaborating with a doctor and found to have the capacity to make health care decisions. Once this determination is made, these individuals are referred to as “mature minors.”
The law only requires that a witness to your Medical Power of Attorney be over eighteen years old. Additionally, the law says that the following people cannot be a witness to your Medical Power of Attorney:
As part of the Medical Power of Attorney your witnesses must sign a statement that they do not fit any of these categories.
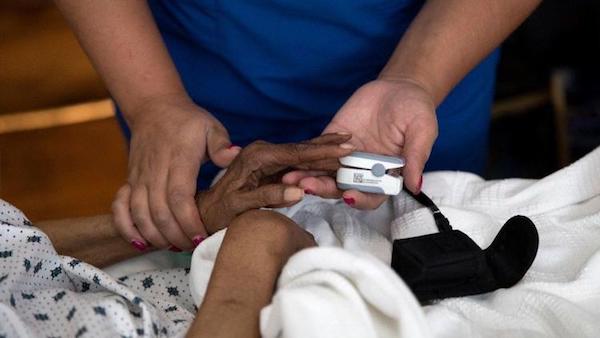
[D]espite confusion over what exactly constitutes “comfort care,” former first lady Barbara Bush’s decision to opt for it is opening doors onto some very important conversations, according to local end-of-life care experts.
Before she died Tuesday, the 92-year-old Bush had been struggling with congestive heart failure and chronic obstructive pulmonary disease, reports said.
When news broke last Sunday that she was opting for “comfort care” during her final hours, a flurry of questions followed.
Is comfort care not medical care? Is it a form of hospice? A form of palliative care?
Janet Burda, advanced practice nurse with Palos Community Hospital’s Home Health program in Palos Heights, said comfort care is a general term for keeping a patient comfortable at the end of life.
“Doing that means providing medical care to help with symptom management,” said Burda, who works with both hospice and palliative care.
Relieving anxiety, pain and shortness of breath are examples of comfort care, she said.
The other part of comfort care, she said, “is helping relieve anxiety for the caregiver.”
Often caregivers don’t know what to expect at the end of a loved one’s life, Burda said, and they often don’t know how to recognize symptoms of discomfort in a patient who is not able to talk or otherwise communicate. “We can help them with that.”
Palliative and hospice care both address the physical, emotional, medical, spiritual and psychosocial needs at a vulnerable time in a patient’s life, she said. They differ, Burda said, in terms of when and where they are applied.
Palliative care can begin at diagnosis, while hospice care is relegated to the last six months of life, Burda said.
Rachael Telleen, director of community outreach programs for JourneyCare, a hospice and palliative care organization that hosts presentations across the region including the south suburbs, said, “Palliative and hospice are both considered comfort care.”
Comfort care, she said, “is a term people are using now because it’s easier for doctors to initiate it.”
The word hospice can really scare people, she said. “So, instead, if we can approach the situation using the word ‘comfort,’ people are more accepting and more open to it.”
Telleen said while both palliative and hospice aim to manage pain and symptoms, palliative care is a support that may be provided while a person is still receiving aggressive treatments.
Hospice, on the other hand, is for patients who are no longer receiving aggressive treatments, she said.
“A patient in hospice receives a lot more services,” Telleen said.
Burda said palliative care allows the patient the option of going back and forth to the hospital. It consists of a team in the inpatient world and a team in the community setting, she said. They work alongside an attending physician.
“A person who has cancer and is receiving chemo or radiation can be under palliative care for symptoms such as pain, anxiety, shortness of breath, nausea, vomiting or diarrhea,” she said.
“A palliative care team can help manage those symptoms but the patient wouldn’t qualify for hospice because they are not necessarily terminal,” she said. “We’re kind of that stepping stone before hospice.”
While palliative care can go on for an extended period of time, hospice is for patients who are expected to live six months or less, Burda said.
To qualify for hospice, a patient must have a qualifying terminal illness and meet certain criteria, Burda said.
“Old age is not a qualification necessarily,” she said.
All of these options are typically covered by insurance and Medicare, Burda said. Hospice is a Medicare benefit and the components — medications, equipment, physician fees — are typically lumped together.
To some people, Burda said, palliative care sounds better, even if it would be more beneficial for them to be in hospice because of its around-the-clock access to a nurse and symptom care.
“But sometimes that scares people. They don’t want to lose that option to go back to the hospital,” she said. “They are not ready to accept that it is the end.”
Sometimes, she said, she walks people through different scenarios to help them picture what the journey will look like.
“At the beginning the patient could be doing fine. That’s the best time to get hospice involved because they get to know the patient and the caregiver and help them on this journey,” she said.
All end-of-life care should begin with conversation, Burda said.
People should take steps to educate themselves and family members about preferences and options, she said. More information on the Palos program can be found here.
“Talk to your family. Have that critical conversation about what you want the end of your life to look like. That affords you the control,” she said.
“There are people who say they don’t know and don’t care. That’s fine too but then designate someone to make those decisions for you when the time comes that choices need to be made,” she said.
Telleen said Bush’s death came on the heels of National Healthcare Decisions Day, which was April 16.
She said the former First Lady’s passing has sparked conversation about end-of-life planning.
“We want people to know what they want before they’re in a crisis,” she said. “Making decisions in a crisis is the most challenging time for people to think clearly.”
Telleen said she encourages everyone older than age 18 to think about advanced care planning and to develop an advanced directive.
“That is being prepared in case something happens and you can’t speak for yourself. And that can happen when you’re 20 or 30. It doesn’t just happen to people who have an illness that is progressing. It could happen because of a car accident. It could happen at any point in an unexpected manner,” she said.
“Ask yourself, ‘If I couldn’t speak for myself who do I identify to speak on my behalf and does that person understand what your wishes would be?’” Telleen said.
Telleen said JourneyCare (https://journeycare.org/) provides a free document called Five Wishes available to residents in 10 counties in northeast Illinois to help them make advanced care decisions. For more information, go to journeycare.org/advance-care-planning.
Complete Article ↪HERE↩!

By Cory Fisher
[D]espite the fact that most seniors have very specific ideas regarding how things should be handled when it comes to their care at the end of life, a surprising number have not shared this information with their offspring.
Too often seniors and adult children are eager to avoid the topic and therefore do not take the steps necessary to plan for the final years of life — including getting financial affairs in order and creating plans for care when a senior’s health inevitably begins to decline.
A new survey by Home Instead, Inc. found that while 73 percent of seniors have a written will, only 13 percent have actually made arrangements for long-term care. Additionally, 79 percent of seniors are more comfortable planning for their funerals than planning for when they need full-time care or hospice.
New research reveals it’s the children who feel the most awkward about broaching the subject of a parent’s final wishes. Even as parents approach their final years, adult children still find it hard to accept their parents’ mortality and believe the topic might be upsetting to parents or grandparents.
Yet once the subject has been broached, a 2017 survey of 505 seniors age 75 and over, and 510 adults between the ages of 45 and 69 revealed something quite different. A whopping 88 percent of seniors said discussing plans for their final years made them feel closer to their adult children, and 97 percent of adults who helped with their parents’ planning said it “gave them peace of mind that things would go okay.”
Those end-of-life fears that lead to avoidance only delay the inevitable. In most cases, adult children will be monitoring their parents’ care and the more information they have, the better.
Research, as well as Home Instead Senior Care experts say there are ways to combat those fears. Talk it out, don’t wait for a crisis, put a plan in place, consult experts on end-of-life issues and follow the “40-70 Rule,” which means that if you are at least 40, or your parents are at least 70, it’s time to start about certain senior topics.
Some of the most common fears experienced by seniors, according to research compiled by Home Instead, Inc., include:
What you can do about it: Consider establishing a living will. Living wills detail an individual’s treatment preferences in the event he or she is unable to make those decisions. Many lawyers will prepare a living will as part of an estate planning package.
What you can do about it: There are many options for end of life care outside of nursing homes and hospitals. Adult children can help their parents research home care options so the entire family is prepared when the time comes.
What you can do about it: It’s wise to have seniors designate a trusted person with power of attorney who will act on their behalf in the event that they are no longer able to advocate for themselves. This will give them peace of mind that their care wishes will be met regardless of their mental acuity.
For adult children, experts suggest the best way to address the end-of-life fears is to communicate clearly with parents about their wishes way in advance. Record specific discussions by taking notes, which could be helpful when making decisions in the future.
For those who feel a great deal of anxiety surrounding this topic, Home Instead offers free resources to encourage seniors and their adult children to talk together about important life plans, which can include end-of-life care, finances, insurance and funeral planning.
A novel component of the free resources offered includes a music generated feature entitled, “Compose Your Life Song.” The light-hearted online exercise, which can be found at http://www.caregiverstress.com/end-of-life-planning/compose-life-song/my-song/, can help families broach difficult subjects more easily.
After completing the activity, seniors are presented with their own customized “song” and accompanying resources that will help them reflect on their personal preparedness during their final years.
The song is a great way to gracefully transition into more serious topics, said Buck Shaw, owner of the Home Instead Senior Care office serving Sacramento, Nevada, Placer and El Dorado counties.
“It’s fun — I’ve done it myself,” he said. “It’s a very basic questionnaire that is a nice blend of topics. It’s so important to talk about these things — I can’t tell you how often I’ve seen families have disagreements when plans aren’t in place. One part of the family thinks grandpa wants one thing, while the other side thinks the opposite.
“It creates an awkward division of the family. I’ve even seen very educated people — doctors and teachers — arguing with relatives who are trying to keep grandpa alive when he was good to go. This can cause rifts in the family that are hard to repair.”
Participants who go online to create their own song respond “yes” or “no” to thought-provoking statements, such as, “I have checked off an item on my bucket list in the past year,” “I frequently visit with people whose company I enjoy,” “I have talked to my family about my end-of-life wishes” and “I have established a will and advanced directives.” This can open the door to deeper, more constructive conversations, said Shaw.
“About 77 percent of adult children think their parents have plans in place, while only 50 percent do,” he said. “In the long run, if we become advocates for seniors, we all win in the end. It’s all about raising awareness and doing the right thing.”
Complete Article ↪HERE↩!