— Toronto ‘death cafés’ offers a new way to get comfortable with that fact

“We’ve heard the saying that it takes a village to raise a child. That village is equally important at the end of our life as it is in the beginning.”
After more than a decade living side by side on a quiet street in Toronto’s east end, Fiona* and her partner Lorraine* had become close friends with their neighbour Tony.
“Lorraine and Tony talked all the time,” said Fiona. “When he started getting older and lived on his own, she helped him with errands and grocery runs. I mowed his lawn.”
When Tony was diagnosed with inoperable cancer in 2018, Fiona started cooking for him and filling in when support workers and nurses weren’t on duty.
When it came to preparing to die, though, the couple decided Tony needed more help than they could offer.
They enlisted the help of a death doula: someone who is trained to help with emotional and physical support as well as education about the end-of-life process.
In the last couple of days of Tony’s life, Fiona slept on the couch next to his bed. The doula and Lorraine sat with him until he died.
What struck Fiona as most remarkable, she said, was the “ceremony of it all.” Lorraine and the doula washed Tony’s body and sat with him for hours after he passed.
“I think, in a lot of western cultures, people don’t want to hang out with a person’s body after they’ve gone,” she said. “This felt like helping him to move on and there was a level of comfort in it that helped all of us.”
Death-care practices vary according to culture and religion, and many doulas argue that in western cultures there’s a lingering taboo around frank talk about death, something that makes it harder for many to deal with death, dying and grieving.
That started to change 20 years ago with the first “death café,” an initiative launched by a recently widowed Swiss sociologist named Bernard Crettaz. The concept — usually a scheduled group discussion about death among people from all walks of life (not to be mistaken for grief counselling) — has since spread and evolved.
“Now there are ‘death salons,’ ‘death dialogues’ and ‘death book clubs,’” said Kayla Moryoussef, who works with Toronto’s Home Hospice Association and has her own practice, the Good Death Doula. “There’s even a ‘death over drafts’ thing where people meet in bars to drink and talk about dying and death.”
Probably the biggest change to the death café model in Toronto has been that, pre-pandemic, the Home Hospice Association’s death cafés were held in bricks and mortar spaces. When the pandemic forced the cafés online and they no longer had to worry about venues and attendance, it allowed the association to offer more niche programming, such as cafés for parents, pet lovers caregivers and “spoonies” (people experiencing chronic pain).
“I came up with the idea for a spoonies death café because, as a person with chronic illness and disability, I know my relationship with dying and death is fundamentally different than my peers, — especially peers my age,” said Moryoussef, who is now in her late 30s.
The mission at the Home Hospice Association is to offer distinct programming for different communities in the name of accessibility and equitability.
“The reason we even got into this death doula training, development and mobilization was because we could see that our health-care system was not going to be able to keep up,” said Tracey Robertson, a doula and co-founder of Toronto’s Home Hospice Association.
Even if our health-care system could bounce back from its current state, most medical training is about finding cures, and many doctors receive little or no training when it comes to talking about death.
“We’ve all heard the saying that it takes a village to raise a child — we always say that village is equally important at the end of our life as it is in the beginning — some may even say more important,” said Robertson.
Death cafés are part of the foundation for that vision, she explained, because you can only build that village after death is normalized and communities are more comfortable talking about it.
“All it requires is for all of us to just get a little bit more comfortable with the fact that we all are going to be there one day,” said Robertson. “How can we help our neighbour who is faced with the reality of sitting in a doctor’s office and hearing words none of us ever want to hear?”
Complete Article ↪HERE↩!
Palliative and hospice care in hospitals and clinics
— The good, the bad, and the ugly
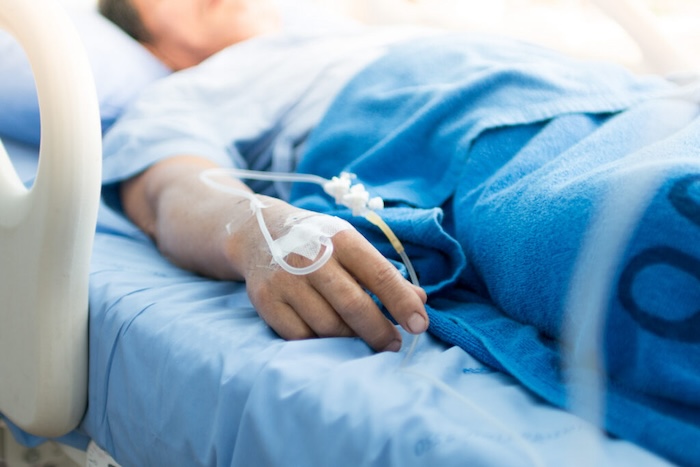
By Earl Stewart, Jr., MD & Miguel Villagra, MD
I walk into the patient’s hospital room during evening rounds. He looks pale and tired, having recently completed a round of chemotherapy for his stage IV pancreatic cancer. His wife is at the bedside, scared and concerned about her husband’s rapid decline. I sit down to discuss goals of care when the patient immediately says, “I can’t do this anymore.” His wife responds immediately to the patient: “Of course you can.” As I delve deeper into the patient’s constant pain and discomfort, the conversation naturally shifts toward a comfort care-focused approach. After 55 minutes at the bedside, both patient and wife agree to further discuss this with the palliative care team. Ultimately, the medical team decided to transition the patient to hospice care.
Similar examples exist in outpatient practice. Take, for example, the 56-year-old female patient with metastatic non-small cell lung cancer who would clearly benefit from early institution of palliative care given the known mortality benefit. When you see her time and again, she engages in candid discussions with you as her physician that she would rather let “nature take its course.” She doesn’t want chemotherapy. She refused radiation. She continues to smoke. She doesn’t want her family to know, and palliative care options, though previously discussed with her, remain out of the question for her.
These are realistic examples from daily practice that present an interesting quagmire to the practicing physician as he or she treads the lines of patient autonomy and applies the evidence of what has been shown to clearly help a patient feel and live better, especially those with terminal illnesses. Tools exist to aid with these difficult conversations, and awareness among the patient, health care professionals, and family members makes all the difference in having these critical discussions. It’s often rather difficult to accept when you are taught to do something but come to the realization that sometimes doing nothing is what a patient prefers. In that moment, you realize that doing nothing means doing everything.
Sometimes practicing hospital medicine is a battle between life and death. Outpatient practice, too, is rife with such battles between the material and immaterial. Palliative and hospice care, though different, offer hope and comfort in some cases. Together, these medical disciplines not only alleviate physical suffering but also, through a conjoined care model, address the emotional and spiritual needs of patients and their families, guiding them through one of life’s most difficult journeys.
Palliative care is a specialized approach that aims to alleviate physical symptoms, manage pain effectively, and reduce the emotional and psychological distress experienced by individuals facing incurable illnesses, irrespective of their specific diagnosis. Palliative care is designed to improve the quality of life for both patients and their families. At the center of this is holistic care. A patient qualifies for hospice services if he or she has an illness that limits his or her life expectancy to six months or less.
Transitioning a patient from palliative care to hospice care is a crucial step that signifies a shift toward comfort-focused end-of-life treatment. Clear communication, compassionate support, and honoring patient and family preferences play critical roles in improving quality of life, increasing satisfaction with care, and enhancing emotional well-being during this transition. This process ultimately hinges on doing what is in the patient’s best interest and ensuring a death with dignity.
Physicians navigating palliative and hospice care face a unique set of emotional and professional challenges, such as handling end-of-life conversations with families to determine a patient’s goals of care, managing pain and symptom control effectively, and addressing spiritual distress in patients. However, within these challenges, there is a profound reward in making a significant difference in the final stages of a patient’s life. It has been previously heralded that caring for the dying patient is indeed a rewarding challenge given the intricacies it presents and doing so is crucially important is physician education. We now know that not only does education matter for physicians in these veins of practice, but it matters for nurses as well.
In palliative and hospice care, an interdisciplinary approach involves physicians overseeing medical decisions, nurses providing direct patient care and symptom management, social workers addressing psychosocial needs, chaplains offering spiritual support, and pharmacists ensuring proper medication management. Each team member contributes his or her expertise to create a comprehensive care plan that supports the physical, spiritual, and psychosocial well-being of the patient, highlighting the power of collaboration in providing holistic, patient-centered care.
Physicians navigating the complexities of palliative and hospice care must adopt practical strategies for effective patient management and compassionate support. Key strategies include fostering open communication with patients and their families, setting realistic expectations, and managing one’s own emotional well-being. Active listening, providing clear and empathic explanations, and involving the entire care team in medical decision-making are crucial for effective patient care.
Though we understand more as a physician community about employing palliative and hospice services for our patients when apropos to providing evidenced-based care, we are aware there is still work to be done to better the delivery of this care.
It has been documented that work is needed to further guide the integration of the family meeting specifically into oncology practice.
Recent data have shown how the institution of information technology and so-called “e-health” methods can be very helpful in individualizing care and extending palliative care services to patients.
We will all have these conversations. We will see patients like these. We charge all physicians to embrace the tenets of palliative care and hospice when appropriate for their patients and to learn more about the services offered in their hospitals, health systems, and practice structures to provide for the most optimal health outcomes.
Complete Article ↪HERE↩!
I understand why people are wary about assisted dying
— But it gave my mother a dignified end

The Dutch legalisation spared her further misery. We don’t take euthanasia lightly; we’re just grateful to have the option
My mother, Jannèt, was 90 years old when she ended her life by means of euthanasia. For years she had been suffering from numerous serious and painful conditions that made her life miserable. She always worried about her health and was terrified of what the future undeniably held in store for her: more pain, more dependence on others, more suffering, more desperation.
On 20 June 2022 at 2pm she was visited by a doctor and a nurse. They had a last conversation with her, during which the doctor asked her if euthanasia was still what she wanted. My mother said yes. She had already decided that she would take the drink herself instead of being injected. She didn’t want to mentally burden the doctor more than necessary.
I was impressed by my mother’s courage in the face of death. She was completely calm, almost cheerful. Before the procedure started, she spoke briefly to us, her three daughters. She told us how it was important to take care of the Earth wisely, to recycle as much as possible and to look after one another. She then drank the small cup in one gulp. She fell asleep very quickly and 15 minutes later the doctor told us her heart had stopped beating. A long and tormented life had come to an end.
The country in which I live, the Netherlands, was the first in the world to legalise euthanasia in specific cases. That was in 2001. Assisted dying has become generally accepted in our country. We talk about it openly and we consider the possibility when situations call for it. We are grateful that this option exists, because it prevents so much pointless suffering. But we never talk about it lightly. Assisted dying has always remained something huge, something you don’t resort to lightheartedly.

As a matter of fact, you can’t. In the Netherlands it will always remain a criminal offence to end a life. Exceptions are made only when a whole range of requirements are met. First of all, the patient must ask for it themselves and must therefore be mentally capable of asking for it. In addition, there are all kinds of due care requirements. For example, the doctor must be convinced that the request for assisted dying is voluntary and that the patient has carefully thought it through. The doctor must also be convinced that the patient’s suffering is hopeless and unbearable. That they can no longer heal, that it is not possible to alleviate their suffering and that there is no reasonable other solution. At least one other independent doctor must be consulted. That independent doctor will discuss the situation with the patient and form his or her own opinion about the situation.
Assisted dying is allowed only if a person is suffering owing to a medical cause, not if someone is simply tired of life or feels that their life is complete. My mother didn’t feel that her life was complete. There were still things that made her happy. She loved flowers and plants; she loved politics; she followed the news. But because of her deafness, incontinence and many other conditions she became socially isolated. Visits from friends became too much for her, and at a certain point even phone calls became impossible.
Walking became very difficult, and she grew afraid to go outside. She always loved to wander through a neighbourhood park, especially in springtime, when the bluebells and lilies of the valley bloomed abundantly. But she was no longer able to go there, not even in a wheelchair. She always enjoyed reading and watching nature programmes, but those things too became increasingly difficult. Her numerous ailments and her lack of mental resilience to deal with them made a normal daily existence impossible. And there was no prospect of improvement.
My mother’s euthanasia was a long process. Five years before her death, she told her GP that assisted dying was what she wanted if her life became unbearable. Over the years, my older sister discussed this wish with her during long conversations. She also took charge of all the conversations that were necessary before permission was finally given.
My mother wanted to celebrate her 90th birthday before she took leave of life. Her last birthday fell on Easter, which she regarded as meaningful. But what kind of birthday gift can you give to someone who will soon be gone? My older sister came up with the idea of making a book in which all her loved ones wrote down what she meant to them, or reminisced. She was very happy with that.
We sat close to her when she died. My younger sister took my mother’s hand and she held it tightly. The older sibling said in a soft voice, “You can close your eyes now, Mum.” That’s what my mother did. I sat there and tried not to cry. It’s not easy to witness your mother drinking a deadly potion and dying after 15 minutes.
The next day was the first day of summer. The sun was shining, the weather was beautiful. I woke up with the pain that my mother was gone. But also with a feeling of relief and deep gratitude that, after such an incredibly difficult life, she had been granted a painless and dignified death. I knew we had given her a great gift.
Complete Article ↪HERE↩!
Ending cancer treatment to focus on living

Alicia Mathlin felt like her body was no longer hers after several rounds of debilitating cancer treatment — so she decided to stop and focus on living her life. Matt Galloway talks to Mathlin about that decision and asks medical experts about the push for ‘common-sense oncology,’ which weighs the pros and cons of certain treatments against a patient’s quality of life.
Matt Galloway cuts through a sea of choice to bring you stories that transcend the news cycle and expand your worldview. It’s a meeting place of perspectives with a fresh take on issues that affect Canadians today.
I’m a death doula
– These are the most common regrets people have before they die
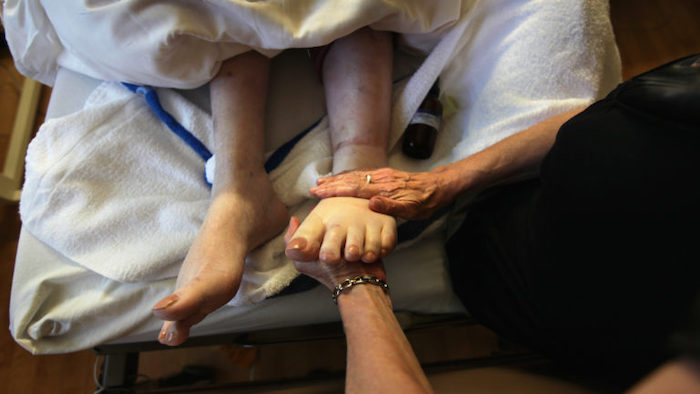
From staying in sexless relationships to putting off downsizing, these are the issues that come up time and time again
There are few as well acquainted with the dying, and their regrets, as death doulas. Also known as end-of-life doulas, they provide support to people through terminal or life-limiting illnesses by improving their quality of life, and death.
This encompasses everything from helping with logistics to providing emotional support to those at the end of life and their loved ones.
i spoke to three death doulas to understand the biggest regrets of the dying, the living who love them, and steps we could take to avoid those same regrets and have a better end of life.
Staying in unhappy (and sexless) relationships
Emma Clare, who is a chartered psychologist and death doula, says that the most common, though unspoken, regret she hears is about relationships.
“I often hear people say that they wish they’d left either unfulfilling or unhappy relationships sooner. A lot of people have regrets about spending a large part of their life in situations that didn’t feel true to themselves or have any fulfilment.”
She says when we’re confronting death, we feel a lack of intimacy and closeness acutely – including sexual intimacy.
“As humans we look for intimacy and that doesn’t go away because we’re dying. If anything, it increases because people are aware they have a limited time left and they want to have that connection with other people.”
Not downsizing or decluttering
“We all know we’re going to die, but we just put it to the side, even with a terminal diagnosis,” says Jane Depledge, a doula based in North Powys, Wales. When patients are told that treatment is going to stop, that lack of preparation “hits them”, she says. Getting a will in place, transferring over health insurance, or discussing their wishes are all simple things that we don’t want to face, but will feel better for it.
Emma Clare adds that this includes very practical decisions.
“People wish they’d downsized their home earlier and cleared out their stuff, and now they’re aware their often adult children are going to have to deal with that and feel a big sense of guilt. That means regret from the family too: they’re then left sorting that out and haven’t had the conversation about what was and wasn’t treasured and should be kept.”
Being in hospital instead of at home
“People often don’t realise they have choices”, says Depledge, so when a person is dying they panic and send them to hospital. Though for some people hospital care is essential, she says it is always worth asking and looking into ways their loved one could die at home.
Not being prepared
The emotional and physical burden of caring for someone at the end of life can take its toll on both the carer and the patient, who may feel huge guilt at being ‘a burden’. People often regret being inadequately prepared for everything that needs juggling, and not realising what support they can get.
“Carers can claim immediate Government grants to care for someone who is dying,” explains Depledge. “Knowing that could have enabled someone to take time off work or give up work to care for and be with a loved one.”
Not being able to say goodbye to friends
When a person is dying, they tend to want to surround themself with the things and people they love most – but so often, they are lonely, says Depledge.
“I think a lot of people avoid visiting people when they get a terminal diagnosis because they worry they don’t know what to say,” she explains. “But actually I hear a lot of upset from the people who are dying, saying that they feel like their friends have gone quiet or disappeared and they feel very lonely. And that’s needlessly lonely because at the funeral there are lots of people there.”
Not saying how you really felt
Amanda Waring, a death doula working in West Sussex says that the biggest regret she comes across is from people who feel they didn’t “heal their relationship, or speak frankly”.
“Regret stems from a lack of honesty. This is true even for exceptionally difficult conversations where someone has wronged the other and the only catharsis is if you bring it into the open and it takes a lot of courage.”
She says this can range from apologising for harsh words spoken at a bedside, to being honest about deeper rooted, historical conflicts, to sharing feelings of love and pride that were perhaps not made clear before.
“Bravely speaking up and trusting your gut is the key to avoiding all regrets really,” adds Emma Clare.
Complete Article ↪HERE↩!
Incurable but not hopeless
— How hope shapes patients’ awareness of their advanced cancer prognosis
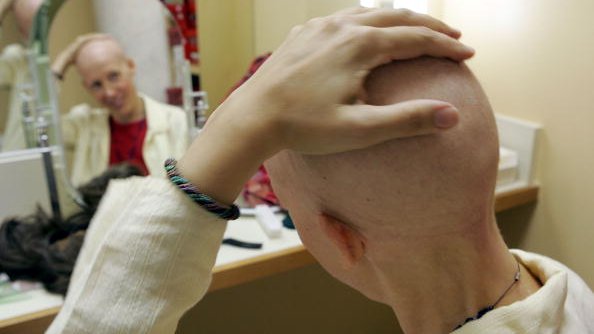
Hope is defined as the expectation of achieving a future good. Patients with cancer, whether it is curable or not, prioritize cure as their highest hope.
Patients with incurable cancer wish to be informed about their disease and its treatment, but also need to maintain hope. This inner conflict can impact how they process information about their prognosis.
Prognostic awareness
Physicians are ethically obligated to inform patients about their prognosis so that patients can make cancer treatment decisions that are consistent with their values. When oncologists talk to patients about prognosis, they tend to talk about the extent of the disease (localized or metastatic), the goal of the treatment (curative or palliative) and the estimated survival (short months or many years).
Communication about prognosis can be challenging due to physician factors such as skill in discussing bad news, and patient factors such as denial. Some patients with incurable cancer, who are aware of their prognosis but haven’t accepted it, will say the treatment goal is cure.
Previous research indicates that less than half of patients with incurable cancer are aware of their prognosis. This is often attributed to a failure of communication.
But are patients truly unaware, or are they aware and not accepting of their prognosis? If inaccurate prognostic awareness is due to denial in spite of adequate communication from the oncologist, then interventions to improve communication may be ineffective, misguided or even harmful.
Patients with incurable cancer are more likely to receive end-of-life care concordant with their preferences when they have accurate prognostic awareness. Inaccurate prognostic awareness can lead to conflicting treatment decision-making between patients and oncologists, delayed referral to palliative care and more aggressive care at the end of life.
In a study of patients with advanced lung cancer, those who received early palliative care and had accurate prognostic awareness were more likely not to choose intravenous chemotherapy in the last two months of life, which would have been futile and worsened the quality of their end-of-life care.
How prognostic awareness is measured
Measuring prognostic awareness in patients is challenging because their responses may reflect their hopes rather than their true beliefs. In a recent publication in the Journal of the National Cancer Institute, our research team synthesized data from 52 studies measuring prognostic awareness in patients with advanced cancer.
In the majority of studies, prognostic awareness was conceptualized as a binary entity: patients were asked if their cancer was curable, and their responses were coded as either accurate prognostic awareness (patients knew their cancer was incurable and responded that it was incurable) or inaccurate prognostic awareness (they thought it was curable and responded that it was curable).
A few studies included in our review improved upon the binary conceptualization by incorporating hope in the assessment of prognostic awareness.
These studies asked patients about their belief and their doctor’s belief about prognosis and found that about a third of patients will hold onto hope for a cure (responding that they believe their cancer is curable), even when acknowledging that their doctors were treating them with palliative intent. This discordance was attributed to poor coping.
The role of hope
Hope is a recognized coping strategy in patients with cancer. However, “false” hope may have detrimental effects. Patients may refuse to believe their prognosis and demand aggressive treatments that may cause more harm than benefit.
In the context of advanced cancer, the relationship between hope and hopelessness is balanced by acceptance, which can re-direct hope to new goals beyond cure, such as hope for connection with others and enjoyment of daily pleasures.
Nurturing hope among patients with cancer and their caregivers is possible and includes coping strategies focusing on what can be done (such as control of symptoms) and exploring realistic goals such as dignity and intimacy. Family and spirituality play an important role in supporting patient hope.
Incorporating patient hope into prognostic awareness
We improved upon the binary conceptualization of measuring prognostic awareness by incorporating patient hope, creating a trinary concept: patients who are aware and accepting of their prognosis; aware and not accepting; or truly unaware.
We propose that patients who are aware and accepting should be offered psychological supports to address any negative effects on mood; those who are aware and not accepting should be offered adaptive coping strategies to support their evolving prognostic awareness; and those who are truly unaware will benefit from interventions such as decision-aids and communication training. Early palliative care consultation may be beneficial at each stage of prognostic awareness.
This trinary conceptualization may guide future research to improve our understanding of the impact of hope in the setting of serious illness and help patients receive the right supports in their cancer journey.
Complete Article ↪HERE↩!
Understanding Hospice Home Care
— A Complete Guide

Navigating the later phases of a loved one’s life may be an extremely emotional and difficult experience. During these difficult times, hospice home care arises as a source of comfort and support, providing a compassionate alternative to typical hospital medical treatment. This specialist care focuses on improving the quality of life for those in the final stages of a terminal illness by giving them the dignity, respect, and peace they deserve at home.
The Essentials of Hospice Home Care
Hospice home care exemplifies a compassionate approach to end-of-life care, providing a beacon of comfort and dignity to those in their final stages of life. Unlike traditional medical treatments geared at curing diseases, hospice care focuses on quality of life, providing comfort and support to both patients and their families. This comprehensive care paradigm is holistic, addressing patients’ psychological, social, and spiritual needs as well as the physical symptoms of their sickness.
At the heart of hospice home care is the dedication to respecting a patient’s choices, allowing them to spend their final days surrounded by loved ones in the familiar comfort of their own home. Pain treatment is an important part of this therapeutic method. Expertly trained healthcare experts work diligently to manage symptoms and reduce discomfort, allowing patients to live as fully and comfortably as possible.
Beyond physical care, hospice home care offers emotional and psychological assistance. Hospice staff provide counseling and grief assistance because they understand that patients and their families are going through one of the most difficult times of their lives. This guarantees that families are not alone in their journey, giving them a shoulder to lean on both during and after the patient’s life.
Spiritual care is also an important component of hospice home care, allowing patients and their families to examine life’s core concerns, make peace with unresolved issues, and, if applicable, strengthen their spiritual connections. This component of treatment is tailored to the individual’s beliefs and desires, with the goal of providing peace and meaning to patients and their loved ones during this momentous life experience.
Hospice care teams are multidisciplinary, made up of doctors, nurses, social workers, chaplains, therapists, and trained volunteers. Each member contributes their knowledge to build a support network that surrounds the patient and their family with care, love, and understanding. This multidisciplinary approach assures that every imaginable need—whether physical, emotional, or spiritual—is met.
In essence, hospice home care represents a paradigm shift in how we see the end of life. It is about appreciating the importance of every minute and allowing patients to spend time with loved ones, reflect on their life, and transition quietly. Hospice home care helps to reimagine the final chapter of life as one of love, respect, and compassion, rather than despair.
Who Can Benefit from Hospice Home Care?
Hospice care is designed for patients who are facing the end stages of a terminal illness, with a life expectancy of six months or less if the disease follows its usual course. However, it’s not just for the patients; hospice care also significantly benefits the families and caregivers by providing them with educational resources, emotional support, and respite care, helping them navigate through their grief and the caregiving process.
The Core Services Offered
The hospice care team typically includes doctors, nurses, social workers, spiritual advisors, counselors, and trained volunteers. They work together to tailor a care plan that meets the individual needs of each patient and family, which can include:
- Pain and symptom management: Focusing on alleviating symptoms and ensuring the patient’s comfort.
- Emotional and psychological support: Addressing the emotional, psychological, and spiritual needs of patients and their families.
- Companionship and daily care assistance: Helping with daily activities and providing companionship to reduce feelings of isolation and anxiety.
- Bereavement support: Offering grief counseling and support groups for families before and after their loved one’s passing.
How to Choose a Hospice Home Care Provider
Selecting the right hospice care provider is crucial. It involves considering factors such as the provider’s reputation, the quality of care, the availability of services, and the level of communication and support offered to families. It’s important to meet with several providers, ask questions, and choose one that aligns with the patient’s needs and family values.
The Impact of Hospice Home Care
The importance of hospice home care to patients and their families cannot be emphasized. This approach to end-of-life care has a significant impact on the quality of patients’ final days because it allows them to remain in the familiar and pleasant environment of their own homes. The environment has a significant impact on a person’s well-being, particularly throughout the final stages of life. Being at home rather than in a hospital allows patients to be surrounded by personal memories, things, and the people they care about, which can considerably reduce the emotional load of facing a terminal illness.
Hospice services provide patients with specialized care that addresses their physical, emotional, and spiritual needs. Pain and symptom control are prioritized to allow patients to interact with their relatives and enjoy their remaining time as comfortably as possible. This level of care empowers patients by offering them a sense of control over their lives and the dignity to choose their own treatment and how they want to spend their final days.
Navigating End-of-Life Care with Compassion and Dignity
Families benefit greatly from the extensive support that hospice home care offers. Going through a loved one’s end-of-life process can be emotionally and physically draining. Hospice care teams do more than just attend to the patient; they also assist families with counseling, respite care, and information about what to expect. This assistance is crucial in guiding families through the complexity of sorrow, loss, and the practical aspects of caring. It also allows the family to focus on being present with their loved one rather than being distracted by caregiving or decision-making.
Hospice home care provides significant support to families, which benefits them greatly. Going through a loved one’s end-of-life care can be both emotionally and physically taxing. Hospice care teams do more than just look after the patient; they also provide families with counseling, respite care, and information on what to expect. This help is critical in guiding families through the complexities of grief, loss, and the practical responsibilities of caregiving. It also enables the family to concentrate on being with their loved one rather than being distracted by caregiving or decision-making.
Component of hospice care cannot be overlooked. Families often find themselves in uncharted territory when a loved one enters hospice care. The hospice team’s role in educating families about what to expect, how to manage symptoms, and how to cope with grief is an essential service that can demystify the dying process and alleviate fears.
In essence, hospice home care profoundly impacts both patients and their families by providing a holistic approach to end-of-life care. It ensures that patients can live their final days with dignity and comfort, surrounded by love, while offering families the support, education, and guidance needed to navigate this challenging journey with grace. This model of care not only addresses the physical symptoms of the patient but also nurtures the emotional and spiritual well-being of everyone involved, making the inevitable transition a shared, supported, and deeply human experience.
Hospice home care displays the power of compassion and dignity in the face of life’s most challenging challenges. Hospice care focuses on comfort and quality of life, guiding patients and families through the end-of-life process with dignity and support. If you or a loved one are considering hospice care, remember that it is a decision that prioritizes love, dignity, and comfort during the most difficult times.
