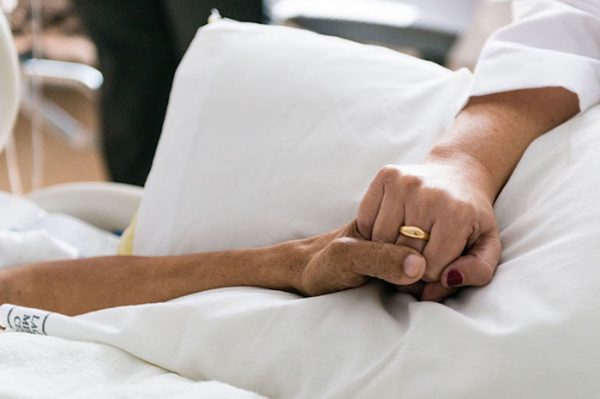
[I]n her last days, 93-year-old Ruth Schroeder lay in bed at Grace Hospice in Regina, slowly dehydrating herself to death because she wasn’t able to die on her own terms.
Schroeder had colon cancer and doctors declined to operate out of fear she wouldn’t survive surgery because of her age — an outcome she’d have been fine with, according to her daughter, Jean Napali, who lives in Vancouver.
Partly that was because of the pain, but also because the painkillers made it hard to concentrate. Schroeder couldn’t really read, watch TV or even do the crossword puzzles she had long enjoyed.
“During the past year she had been making it very clear that she really was done,” Napali said.
Schroeder had talked with her family about ending her life, and with any doctor who would listen while she was in palliative care at Pasqua Hospital in June; she had followed the development of federal legislation for medical assistance in dying (MAID), which was passed by the Liberal government that month.
However, she then learned she had little time left.
“At that point mom felt very relieved that she only had three months to live and she kind of dropped talking about MAID because she was like, ‘There is going to be an end to this, maybe it’s not the route that I need to go,’ ” Napali recalled.
Schroeder lived at home for as long as she could over the summer, cooking her own meals and doing her own laundry with support from her children and a housekeeper. On Aug. 1, she fell in the middle of the night, aggravating the nerve centre on which her tumour lived; the lightest touch on her leg became excruciating. After two days in an emergency room, she was moved to the hospice.
Napali is a mental health worker and her sister was a longtime nurse, so they were able keep their mom off drugs that harmed her quality of life. This included an anti-depressant Schroeder’s palliative team put her on after she expressed interest in MAID, Napali said.
The siblings feel their mother wasn’t taken seriously because of her age.
“As a family we were really floundering, trying to figure out how to put this in place. And it wasn’t until after she had died that we realized she could have signed the forms at the end of June when she was talking with the doctors about it and started the whole procedure,” Napali said.
When Schroeder told her she would stop eating and drinking, Napali called her mom’s doctor about ending her life. However, the doctor wasn’t available for a week. When she did arrive, Schroeder’s painkillers had been increased so much that while she knew her own name, she didn’t know the month and said the year was 1976 instead of 2016. The doctor deemed her not competent enough to consent.
“That upset us quite a bit because it was very clear that she was going to be in a lot of pain — that she was in a lot of pain — and that basically she would just be dehydrating to death over the next few days or weeks,” Napali said.

The federal legislation does not allow for people to give advance consent, when drugs don’t cloud their judgment, for medical assistance in dying.
Because Schroeder wasn’t on any life-prolonging medications she could stop taking, it took her 16 days to fatally dehydrate.
“Somehow to me, that seems wrong, that she needs to suffer through that,” Napali said.
“If a dog was kept in a vet’s office to dehydrate to death for two weeks, everybody would be totally up in arms and be calling it inhumane. And that vet would probably lose his license. And yet for a person, that’s deemed acceptable,” she said.
“It was just really hard for us because as her children we knew what Mom wanted. She was ready to go and she wanted MAID but that wasn’t something that could happen for her. I don’t want other people to have to go through what we went through in terms of not having out mom’s wishes done.”
Aside from the roadblock imposed by the law, Napali was never clear on whether her mother’s doctor even agreed with MAID, and has come to believe most doctors in Saskatchewan won’t perform it.
“I think doctors need to be really clear as to whether they are willing to go that route or not, and if they’re not they need to pass their patient on to somebody who is willing to take a look at that.”
The Saskatoon Health Region is considering a policy to protect the identities of health care providers who participate in medical assistance in dying, fearing that otherwise no one would be willing to provide the service.
The Saskatchewan Medical Association was unable to find any doctors who participate in MAID and were willing to be interviewed for this story.
SMA president Intheran Pillay said some doctors are in favour of MAID, but others object and feel palliative care should be improved, believing that some requests stem from a lack of it. There’s no way of knowing what that split is, he said.

Health care workers who provide abortions in the U.S. have suffered violence, and some fear similar retaliation around MAID, he said.
Some physicians may work in facilities such as Catholic Health Association hospitals which oppose MAID, and don’t want their beliefs public. Others don’t want their patients to distance themselves if they have different viewpoints, he said.
A person’s primary point of contact for MAID should still be their doctor, who can discuss all options to improve pain control and comfort, he said.
“In a majority of cases we’re able to keep the patient really well controlled with regard to pain. I’ve never, in the 24 years I’ve been in practice, had a problem in terms of referring patients to the appropriate specialist to get that patient the care that they need to make them comfortable.”
People seeking information can look up the websites of the College of Physicians and Surgeons of Saskatchewan, the Canadian Medical Association, the SMA and the Saskatchewan government, he said. SHR this month approved its MAID policy, which includes a decision-making guide.
Eight people in the province have received MAID since the legislation passed, according to the health ministry.
Complete Article HERE!