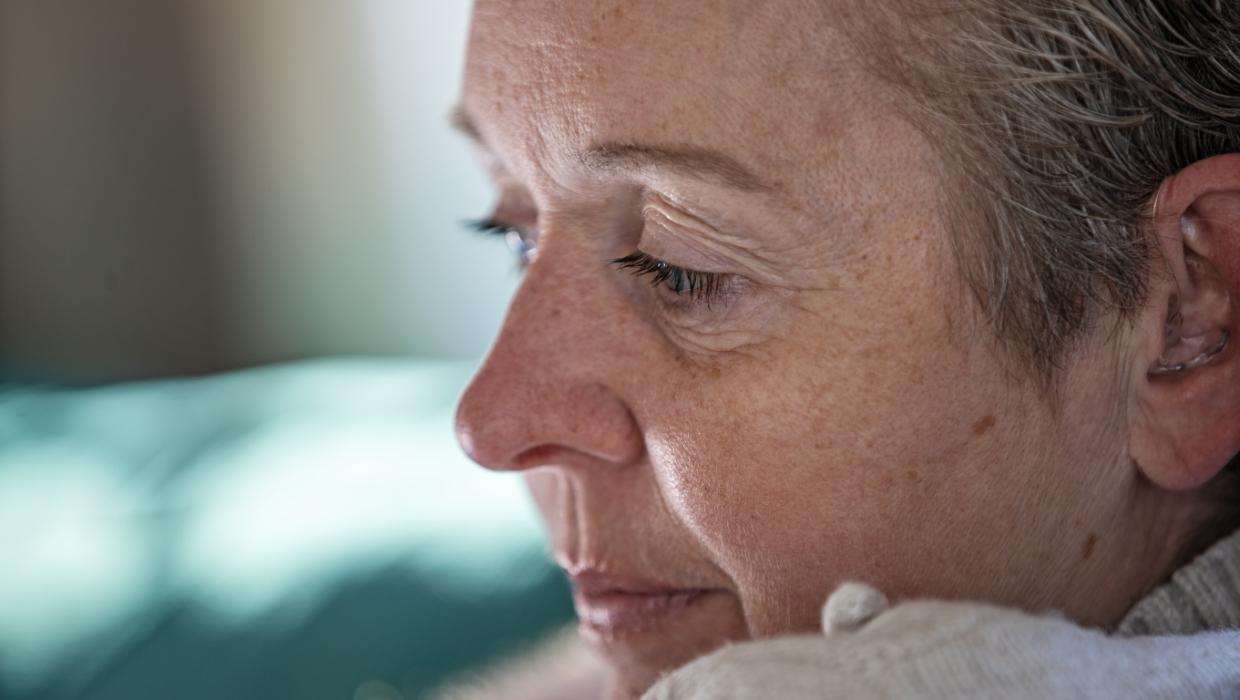
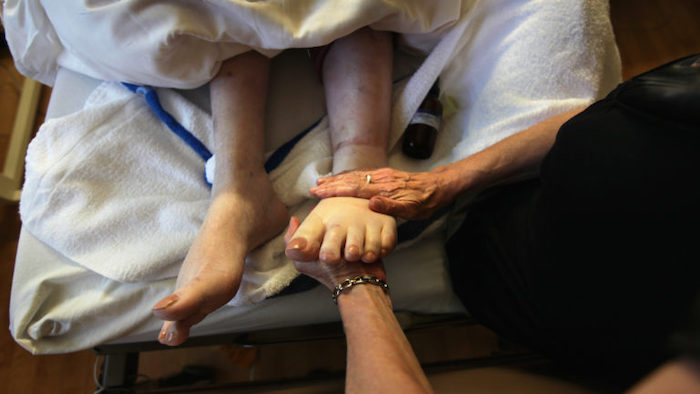
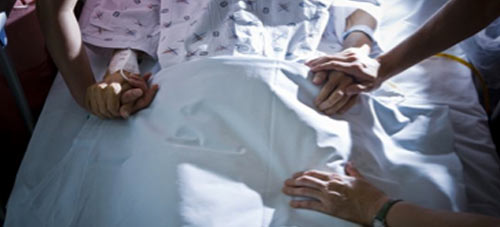
— A Hospice Nurse Works to Change the Conversation on Death
By Jim Parker
Misconceptions about and limited awareness of hospice are among the industry’s largest headwinds, a problem that one hospice nurse in California is working to solve.
Julie McFadden entered the nursing profession 16 years ago, starting her career in intensive care units. After about eight years in the ICU, she “took the leap” into hospice nursing and hasn’t looked back.
More recently, McFadden has begun to take her passion for hospice care beyond the bedside. She has been releasing educational videos on social media platforms and YouTube in which she discusses key aspects of hospice care, terminal illness, caregiving and the dying process. She has more than 47,000 subscribers on YouTube alone, with some videos attracting tens or hundreds of thousands of viewers.
McFadden is also the author of the forthcoming book, Nothing to Fear: Demystifying Death to Live More Fully, slated for release in June.
Hospice News sat down with McFadden to discuss her educational mission, the knowledge gaps she is working to fill and how common beliefs and attitudes about death impact patients and families.

You’ve said you wanted to change the way we think about death and dying. What in your view does need to change?
It seems like everybody, including other health care workers sometimes, thinks that death is the worst possible outcome. So let’s avoid it at all costs, even though it’s inevitable for all of us. And I think that’s a disservice.
The advances we made medically had been amazing, and they do keep us alive much longer. We live better, healthier lives. That’s all amazing. But I think we try to ignore the fact that there is an end point to our lives, so we avoid it at all costs. We think it’s the worst possible thing that could happen, and I think that causes a lot of undue suffering. And suffering to me is far worse than death.
I want to help people see — if death is inevitable — why and how we can better prepare ourselves, so it doesn’t have to be this horrific, traumatic thing.
What was the transition like when you went from the ICU to hospice care? Was there a degree of culture shock? How did you acclimate yourself to that environment?
Yes, there was definitely a degree of culture shock. I had been very unhappy as an ICU nurse for many years, and I just sort of stuck with it thinking it was a “me” problem — that I just wasn’t meant to be a nurse, and I wasn’t a good nurse. There must be a reason I don’t like this. And then when I made the change, I was kind of healing from that.
I do feel like it was kind of traumatic to be an ICU nurse, at least for me. Hospice was a slower pace. I was in people’s homes. There was a lot of autonomy, which is good and bad. And it just took me time to see that I didn’t have to hurry up and care. Like a lot of times in the ICU, it felt very rushed, and I hated that feeling. I felt like I couldn’t care as much as I wanted to, because I was always in a hurry and very task oriented.
In hospice, it didn’t feel like that to me. So it was just a transitional shift. The first year I was getting used to that. And then as I watched all these people die what I would call a natural death, seeing how the body was really taking care of that person, with or without my help, was so fascinating to me. That’s what really got me thinking like, wow, this is a whole new ballgame that I never even knew was there.
Even as an experienced ICU nurse, I feel like I didn’t understand the scope of how our bodies really take care of us, even at the end of life.
Can you expound on that a little bit? What are some of the ways that our bodies take care of us?
For example, almost everyone wasn’t hungry, wasn’t eating and drinking, and they were sleeping a lot of the time. I would hear from my hospice doctors that this is happening a lot of the time because their calcium levels are rising. When you start getting towards the end of life, your body knows it. So it starts like turning off that hunger and thirst mechanism in the brain, because it knows that it doesn’t really need that anymore.
Your body just needs almost like a cocoon. So although there may be some symptoms, because of the disease you’re dying from — it’s not all roses and daisies — in the actual act of dying, the body will start changing chemically. Calcium levels rise; certain things will kick in, and the more that happens, your body can go into ketosis or it can release endorphins or stall pain and give you a euphoric feeling. So there’s many things that just naturally happen.
Could you say more about why the education you’re doing is necessary? What is the knowledge gap you’re trying to fill?
Generally speaking, we have a lot of holes in our health care system. Health care workers don’t have a lot of time. Not everyone has the time to really sit down and educate about a difficult topic like end of life, or the fact that they’re even getting close to the end of life. That’s a difficult thing to bring up.
We’re missing the ability to take that time and space to allow people to hear what’s truly going on and educate them about that. That’s a big missing piece.
In my nursing education, I do not think I learned about death. It was always about keeping people alive. It seems like almost all health care education is about how we keep people alive. So there’s a gap there too, even with other health care workers. So I just felt like, “Why not try to educate the masses in a general way just so they have an idea of what’s going on?” It’s also giving them a way to openly discuss things.
As an ICU nurse, I didn’t know some of the things that I know now as a hospice nurse. There’s a lack of knowledge among health care workers, and definitely lack of knowledge among people who don’t work in health care, which is not their fault. It’s just that we don’t teach or talk about what the end of life is like, and that’s what I’m trying to change. We do need to start talking and planning for it.
I noted some of the some of the videos were sponsored by [the virtual mental health care platform] Betterleave. How did that relationship come together?
I don’t have a manager or an agent or anything like that. Companies just come across my videos. I don’t mind coming into relationship with companies as long as I feel like it’s something I would get behind whether I was paid for it or not.
BetterHelp to me is like such a great concept. So they reached out to me, and because I’m into them, I said, “Yeah, let’s partner.” I have intermittent sponsorships from a company called the Macy Catheter, and then occasional other sponsorships.
You’re still working as a hospice nurse. Is your employer giving you any feedback on your videos? Have they seen them?
I’ve done it for three years now, and I think I was keeping it pretty quiet. I had an article that went really viral almost three years ago, and that’s when they called me into the office. They were happy for me. I love my employer. But we had to talk about what was going on and disclose it to HR to make sure that everything’s Kosher.
I have guidelines I have to follow, which I do as far as HIPAA regulations and not talking about where I actually work. But overall, they’re super supportive.
Complete Article ↪HERE↩!