A sociologist explains how to get the most out of the final months of life
We are all going to die — and most of us will be able to see death coming, months or even years before it happens. That foreknowledge means we should embrace the end of life as a distinct life stage, just like childhood, adolescence and maturity, says Deborah Carr, a sociologist at Boston University. In the 2019 Annual Review of Sociology, Carr and her co-author, Elizabeth Luth of Weill Cornell Medicine in New York, explore how to make the most of this final stage in our lives.
Carr spoke with Knowable about how to find a good death. This conversation has been edited for length and clarity.
You claim that the end of life is a life stage that’s unique to the modern world. Why do you say that?
In past centuries, people tended to die younger, but more important, they tended to die quickly after they became ill. The end of life was basically a week, if that. People died at home. Today, with people dying of conditions like dementia and cancer, someone can experience a month or 10 years between diagnosis and actual death. And today, ventilators and feeding tubes allow people to prolong the length of their life, even if not the quality of life. So it’s a longer and more uncertain stage than in the past.
Is it fair to say that the objective of the end of life is to find a good death?
I think that is one of the main objectives. And that’s a new construct. In the days when people died suddenly, death was really a discrete event. You didn’t have to find ways to soothe them or provide music or other amenities. Today, because people tend to die over prolonged time periods, there’s a real emphasis on ensuring that the quality of that experience, whether it’s a week, a month or six months, is as positive as possible.
What are the components of a good death?
A good death typically has several pillars. First and foremost is freedom from pain. A sizeable portion of dying patients have physical pain and difficulty breathing. So the use of painkillers, palliative care, devices that allow someone to breathe comfortably, is very important.
Another is self-determination. Dying patients and their families want to have some control over the process. They want to choose where they die: at home or in a hospital. They want to choose what kind of treatment they get, whether they get life support.
And the third pillar is a broad category called death with dignity. People want to be treated as a whole person. They want their spiritual and psychological needs met. People even think about planning a funeral that has their favorite music and foods. They want to die being the human being they were in their younger years.
Are there socioeconomic factors that affect access to a good death?
A good death, like a good life, is often a matter of socioeconomic privilege. There are stark race differences in satisfaction with pain treatment at the end of life. There are a lot of explanations for that, but one is discriminatory practices in prescribing painkillers.
Economic factors probably matter most for advance care planning. Low-income people don’t tend to have living wills. One of the main reasons is they can’t afford a lawyer, or they don’t go to a lawyer for a property will because they don’t own a home. Usually it’s when you go to make a will that the lawyer asks if you would like a living will as well.
Socially isolated people are especially vulnerable to a bad death. Family and loved ones are critical in advocating for quality care, for ensuring that one has a clergy person by their side, getting help, making decisions in a sensible way. That’s a lot more difficult for those who don’t have a spouse or child or close friend nearby. So social isolation is a risk factor for a low-quality death.
This is a life stage that most of us will pass into, and we can only do it once. What can we do to make it as good as possible?
Data show that as people get closer to death, they often change their minds about things. Their values change, they start to value things like comfort, spiritual comfort, relationships with family, and they stop fighting. There’s less of a desire to live longer, and more to live better. People need to think about priorities, think about what’s important to them and their families, and adhere to their values, whether personal or religious. That really guides a lot of decision-making. Open and honest communication, along with formal preparations like advance care planning, are healthy approaches that bring both patients and their families peace.
Families and patients can prepare for the end of life by doing things like writing a living will, and specifying what kind of treatment plan one wants, even specifying how much money to leave behind for one’s children and one’s spouse. All of that planning is guided by some sense of when one’s end is coming. That’s why it’s really important that doctors try to give some estimate of how long someone’s future lifespan is. But that’s very hard to do, both psychologically and technically.
The other thing is to communicate with the people close to you. People need support, both practically and emotionally. They need people to talk to, and literally to hold their hand, but they also need people to help them with decision-making, financial decisions, figuring out whether they’re going to spend their last week at home or in a hospital. That communication can be very helpful.
What is society doing right today?
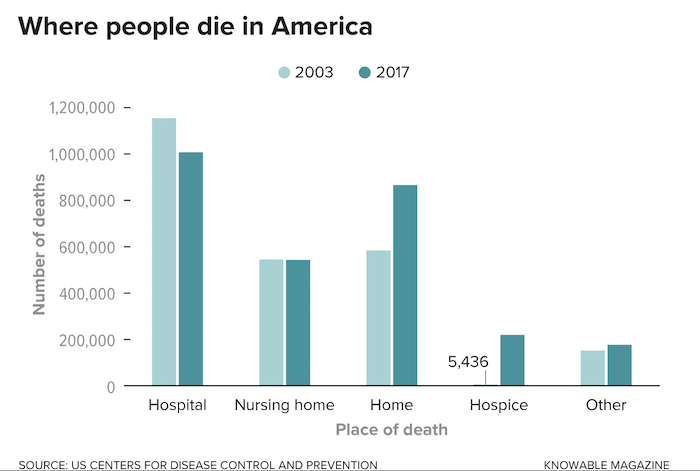
We have rising numbers of people using hospice, which emphasizes soothing of pain and palliation, rather than treatment. I think that’s a real advance. Patients and family members who receive hospice care are almost uniformly positive about the social support they receive.
The proportion of Americans who have living wills, or who appoint a family member to be decision-maker, has skyrocketed. And under the Affordable Care Act, doctors are reimbursed for the time they spend discussing end-of-life issues with their Medicare patients. That’s really important, because doctors are so rushed today. Being reimbursed to take the time to ask older patients what they want has been another real advance. Some private insurance plans cover end-of-life discussions and others don’t. But nearly all older adults in the United States have Medicare, so in practice, nearly all older adults have this benefit. People under age 65 with a permanent disability also may qualify for Medicare, and consequently are eligible for this benefit.
What are we doing wrong?
Despite all the positive trends, there are still millions of Americans who do not take steps to prepare adequately. It goes back to fear and discomfort about death. People are afraid to talk about these issues — they may think “Oh, it looks like I’m after my mom’s inheritance if I talk about it.” But these are conversations that everybody needs to have. Just like parents should have the drug conversation, people should have the death conversation, to talk about their hopes for what they will experience at the end of life. You aren’t going to achieve what you want unless you articulate it to people who can help you sort it out.
If we can normalize and destigmatize death, and recognize it as a normal part of life and aging, that will empower people to discuss these difficult issues.
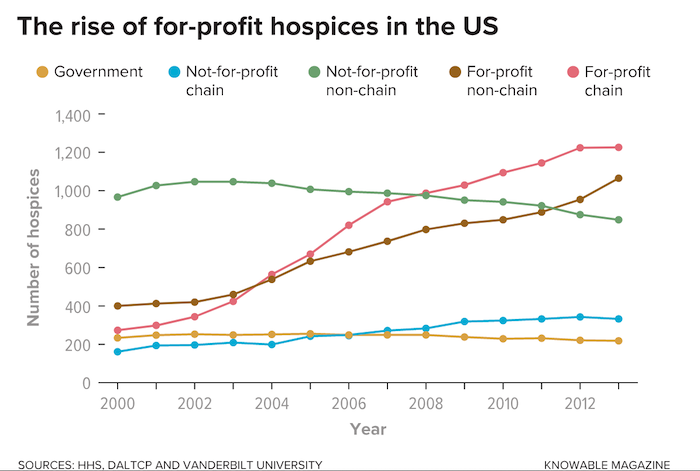
The other problem is that for all the strengths of hospice, the number of nonprofit hospices has been diminishing dramatically, and the number that are for-profit has been increasing dramatically. The people who work for hospices are for the most part kind and loving workers, but the for-profits are motivated to make money, so they’re often treating only the patients who are less expensive to treat. They’re often not delivering care to rural residents who need a lot of travel time. They’re shifting hospice care to nursing homes, because that’s cheaper. But that means fewer people are given the opportunity to die at home if they wish. The move to for-profit hospice is undermining the quality of care, and it’s limiting who gets that care.
So far, we’ve been talking about the needs of people at the end of life. But does the final stage of life offer opportunities as well?
One is the opportunity to construct a “post-self,” the self people want to live on after they die. You often hear that people want to leave the world a better place. End of life is a time when they can really think about what kind of legacy they want to leave behind, whether it’s financial or emotional or social.
It’s also one of those rare opportunities to be wholly introspective. There’s long been a theory that as we get older we care less about possessions and the larger social network, and want to spend our final days dedicating our energy to those people who are nearest and dearest to us. This is an opportunity to show gratitude towards loved ones, to focus on spiritual needs, review one’s life and give love and support to those you’re going to leave behind. It’s sometimes important for dying people to tell family members, “I’m ready to go now, and you can be OK with it.” Having those difficult conversations can make people feel more prepared for the transition.
What are the areas we need to work on in the future?
A big one is physician-assisted suicide and euthanasia. That’s not something that’s taken hold in the US. There’s certainly attitudinal support for it — all the survey data show that people think if someone’s terminally ill, with no chance of recovery, and of sound mind, they should be given the option for euthanasia. I think that’s going to be one of our big questions over the next 10 years about end-of-life care.
Complete Article ↪HERE↩!

