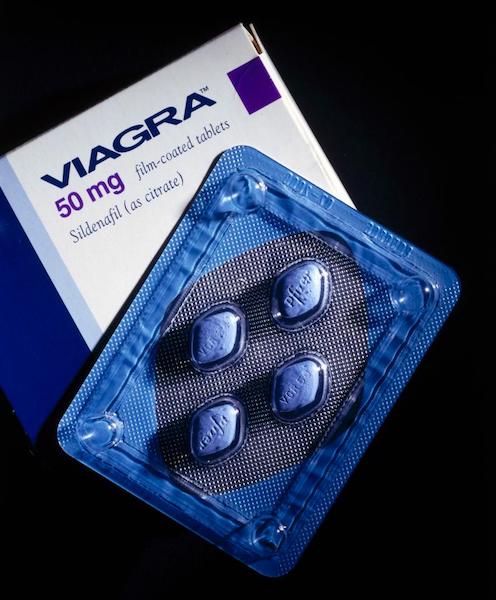
[T]wo years after an abrupt price hike for a lethal drug used by terminally ill patients to end their lives, doctors in the Northwest are once again rethinking aid-in-dying medications — this time because they’re taking too long to work.
The concerned physicians say they’ve come up with yet another alternative to Seconal, the powerful sedative that was the drug of choice under Death with Dignity laws until prices charged by a Canadian company doubled to more than $3,000 per dose.
It’s the third drug mixture recommended by the doctors whose medication protocols help guide decisions for prescribers in the six U.S. states where aid-in-dying is allowed.
“[Twenty percent] of the cases were three hours or more before death, which we think is too long,” said Robert Wood, a retired HIV/AIDS researcher who volunteers with the advocacy group End of Life Washington, in an email. “The longest was 31 hours, the next longest 29 hours, the third longest 16 hours and some eight hours in length.”
Patients and families are told to expect sleep within 10 minutes and death within four hours. When it takes far longer, family members get worried, even distressed, said Dr. Carol Parrot, a retired anesthesiologist who has prescribed drugs for dozens of aid-in-dying patients in Washington.
The doctors say this can be addressed with larger doses of the three drugs they have been using — diazepam, often used to treat anxiety; digoxin, used to treat heart issues; and morphine, a narcotic pain reliever — plus another heart medication, propranolol, in a four-drug cocktail aimed at quickly inducing death, Wood said.
Parrot and Wood are part of a seven-member group of doctors in the Northwest who came up with the three-drug protocol after Valeant Pharmaceuticals Inc. acquired the rights to secobarbital, known as Seconal, in 2015 and raised the price sharply.
“We wanted the new drug regime to be safe, reliable and effective — and cost $500 or less,” said Parrot.
How long until death?
Since 1997, when Oregon’s Death with Dignity law became the first in the nation, doctors had relied on fast-acting, relatively inexpensive barbiturates — either secobarbital or pentobarbital — for patients with terminal diagnoses who sought aid in dying in Oregon, Washington, California, Colorado, Montana and Vermont. The practice also has been approved in Washington, D.C., but is being reviewed by Congress.
Pentobarbital became unavailable after drugmakers blocked its use in U.S. death-penalty executions.
Concerns about the overly long deaths surfaced last summer, Parrot said. Nearly all of the problems occurred in patients already taking high doses of opiates.
“We run into patients who are so tolerant or dependent on narcotics that even the astronomically high doses of oral narcotics in our prescription do not stop them from breathing,” she said.
If patients have diseases that slow or alter normal organ function, it can affect the speed and amount of drugs absorbed in the small intestine, metabolized in the liver and sent to the rest of the body. Very large patients, too, may require larger doses.
Deaths aren’t required to be supervised, and no doctor was present with the unidentified patient who took 31 hours to die, so doctors would only be speculating about the reason, Parrot said.
Not all patients — or doctors — experienced overly long deaths with the previous drug mixture. Dr. Lonny Shavelson, a Berkeley, California, physician who has supervised two dozen aid-in-dying deaths under California’s new law, said it worked fine.
“My personal experience is, I haven’t had long deaths with it,” Shavelson said.
And not all doctors think long deaths are a problem. In Oregon, even with fast-acting barbiturates, time to death has ranged from one minute to 104 hours during the 20 years the law has been in effect, state records show.
“I’ve heard stories where it took quite a number of hours to die, and it was fine,” said Dr. David Grube, an Oregon-based medical director for the advocacy group Compassion & Choices.
Scrabble, then lethal drugs in scotch
Scott and Amy Kreiter, of Wenatchee, didn’t know what to expect when Scott’s mother, Patricia Hansen, 69, decided to take the lethal drugs on Dec. 26, 2016. Hansen, a lively woman who once ran a gourmet ice-cream business, had endured frequent hospitalizations for end-stage kidney failure, congestive heart failure and other ailments.
“She said, ‘I want to listen to Willie Nelson, I want to play a game of Scrabble, I want to drink a Rob Roy or two, and then I want to be done,’ ” said Scott Kreiter, 47.
Hansen proceeded to “kick our butts” at Scrabble, her son said — including fulfilling a goal of getting a triple-word score with a dirty word. Then she mixed the drugs with scotch and drank the solution.
“She didn’t complain. She just took it,” her son recalled. “She said, ‘You thought I’d chicken out, didn’t you?’ ”
Within two minutes of downing the mixture, Hansen was asleep. Within 20 minutes, her breathing had stopped.
“We thought it would take one to two hours,” Amy Kreiter said. “It if had gone on for hours, we would have thought we did it wrong.”
Critics of aid-in-dying say growing reports of overly long deaths underscore their objections. Dr. David Stevens, CEO of Christian Medical & Dental Associations, which has tried to halt or reverse laws, said coming up with new drug protocols could eventually be a step toward Holland’s practice of allowing euthanasia by lethal injection “so the patient could be killed ‘humanely.’ ”
“We are heading down that same path,” Stevens said in an email.
But Parrot and other frequent prescribers of aid-in-dying drugs say they are looking for the best way to honor the wishes of patients in states where the practice is allowed. Doctors recently began using the newest drug mixture and will gather data about its effectiveness.
“We’re not experimenting,” Parrot said. “We are working with available drugs to provide dying patients a comfortable, peaceful death that is reliable and safe for them and comforting for their families as well.”
Complete Article HERE!

By Andrew M. Seaman
[O]bese people in the U.S. may not receive the same kind of care at the end of their lives as people who are thin or normal weight, suggests a new study.
Before they died, obese patients were less likely to enroll in hospice care, spent less time in hospice and were less likely to die at home than thinner people, researchers found.
End-of-life care was also more costly for obese people.
“People with obesity deserve high-quality care, but may not be receiving it at the end of life,” said lead author Dr. John Harris, of the University of Pittsburgh School of Medicine in Pennsylvania.
More than a third of U.S. adults are obese, according to the U.S. Centers for Disease Control and Prevention.
Harris and his colleagues note in the Annals of Internal Medicine that aside from health risks, obesity may present technical and logistical challenges during physical examinations and certain medical procedures.
Previous research also shows that stigma about weight affects how doctors and patients behave, they write.
To see how body weight is linked to healthcare at the end of life, the researchers used data collected between 1998 and 2012 from 5,677 people on Medicare, the U.S. government’s health insurance program for the elderly and disabled.
None of the participants were living in nursing homes or other institutions. The data were drawn from the last six months of their lives.
Based on body mass index (BMI), a measure of weight in relation to height, 7 percent of participants were underweight with a BMI of 18.5 or below, 44 percent were normal weight with a BMI of 18.5 to 24.9, 31 percent were overweight with a BMI of 25 to 29.9 and the rest were obese or morbidly obese with a BMI of at least 30.
A 5-foot-5-inch person weighing 120 pounds would have a BMI of 20, in the normal range. A person of the same height who weighed 240 pounds would be morbidly obese, with a BMI of about 40. The National Heart, Lung and Blood Institute provides a BMI calculator online (bit.ly/2lHXqP2).
The researchers found a 38 percent probability that people with a BMI of 20 would enter hospice care toward the end of life, compared to about 23 percent among people with a BMI of 40.
Hospice care, which can be provided in home or at a facility, provides physical support, including pain control, and emotional support for patients and families dealing with terminal illnesses.
When people with a BMI of 40 did receive hospice care, it was typically for a shorter time than normal-weight people.
“It’s looks like people weren’t getting enrolled, and they got there later if they were enrolled,” Harris told Reuters Health.
The researchers also found that obese people had lower odds of dying at home, which is a typically a wish for people at the end of life. Their likelihood of dying at home was 55 percent, compared to 61 percent for normal-weight patients.
Gaps in care generally rose as BMI increased, the researchers found.
“It seems like people with obesity are getting lower quality of care at the end of life,” said Harris.
The cost of care was also higher when BMI was higher, they found.
The study can’t say why these gaps exist, but the researchers suggest it may have to do with obese people looking less gaunt toward the end of life and not being referred for hospice. Or, they may be unable to find a hospice program that can accommodate their healthcare and family’s needs.
The healthcare systems needs to make sure it’s offering everyone the same level of care, said Harris.
His overarching goal, Harris said, is to improve the quality of care for people with obesity.
Complete Article HERE!
The time between diagnosis and death presents an opportunity for “extraordinary growth.”
By Emily Esfahani Smith
[T]he psychiatrist William Breitbart lives at the edge of life and death. As chairman of the Department of Psychiatry and Behavioral Sciences at Memorial Sloan Kettering Cancer Center in New York, Breitbart specializes in end-of-life care for terminally ill cancer patients. For many of his patients, the most pressing question isn’t when they’ll die or how painful death will be. Rather, it’s what makes life meaningful. They are in search of a meaning that cannot be destroyed by death.
Is there one?

Breitbart has spent the better part of his career trying to answer that question. His ground-breaking research shows that while the specter of death often leads people to conclude that their lives are meaningless, it can also be a catalyst for them to work out, as they never have before, the meaning of their lives.
When people believe their lives are meaningful, according to psychologists, it’s because three conditions have been satisfied: They feel their existence is valued by others; they are driven by a sense of purpose, or important life goals; and they understand their lives as coherent and integrated. Psychologists and philosophers say that the path to meaning lies in connecting and contributing to something that is bigger than the self, like family, country, or God.
Meaning and death, Breitbart believes, are the two sides of the same coin—the fundamental problems of the human condition. How should a human being live a finite life? How can we face death with dignity and not despair? What redeems the fact that we will die? These questions roll around Breitbart’s mind every day as he works with patients facing life’s end.
Breitbart’s interest in meaning took root in his childhood. Born in 1951, Breitbart grew up on the Lower East Side of Manhattan. His parents, Jews from eastern Poland, narrowly avoided Hitler’s death camps. When they moved to America, they carried their memories of the war years with them. Breitbart’s childhood was steeped in that tragic past. Every morning, his mother would ask him at the breakfast table, “Why am I here?” Why, she wondered, did she live when so many others had died?
“I grew up with a sense of responsibility to justify my parents’ survival and to create something in the world that would be significant enough to make my life worthwhile. It’s no coincidence,” he laughed, “that I ended up at Sloan Kettering.”
Breitbart began working at the hospital in 1984 during the height of the AIDS epidemic. Young men his age were dying all around him. As he tended to them, “They were constantly asking me to help them die,” he said. He was also working with terminal cancer patients. “When I walked in the room, they would say, ‘I only have three months to live. If that’s all I have, I see no value or purpose to living.’” They told him, “If you want to help me, kill me.”
If death means non-existence, Breitbart’s patients reasoned, then what meaning could life possibly have? And if life has no meaning, there’s no point of suffering through cancer.
By the ’90s, physician-assisted suicide was a hot topic in Breitbart’s circles and beyond. The doctor Jack Kevorkian had helped his first patient end her life in 1990. As the United States debated the ethics of assisted suicide, other countries were taking steps toward normalizing the practice. In 2000, the Netherlands became the first nation to make physician-assisted suicide legal. Today the practice is legal in the United States in California, Vermont, Montana, Washington, and Oregon.
As Breitbart heard more stories of assisted suicide, he began to wonder what specifically was driving the terminally ill to give up on life. At the time, he was doing research studies on pain and fatigue at the end of life, so he tacked onto those studies some questions that asked his subjects whether they felt a desire for a hastened death. What he discovered surprised him.
They no longer wanted to die. Their spiritual wellbeing improved. They reported a higher quality of life.
The assumption had been that the ill chose to end their lives because they were in terrible pain. But Breitbart and his colleagues found that wasn’t always the case. Instead, those who desired a hastened death reported feelings of meaninglessness, depression, and hopelessness. When Breitbart asked patients why they wanted a prescription for assisted suicide, many said it was because they had lost meaning in life. Unlike clinical depression, which has a specific set of diagnosable symptoms, meaninglessness was more of an “existential concern,” Breitbart said—a belief that one’s life has little value or purpose and is, therefore, not worth living.
Breitbart knew he could treat depression—there were medicines and well-developed psychotherapies for that—but he was stumped when it came to treating meaninglessness. Then, in 1995, he began to see a way forward. He was invited to join the Project on Death in America, which aimed to improve the experience of dying. Breitbart and his colleagues on the project—including philosophers, a monk, and other physicians—had long conversations about death and the meaning of life, “peppered with references to people like Nietzsche and Kierkegaard and Schopenhauer,” Breitbart said. “What I suddenly discovered,” he explained, was that “the search for meaning, the need to create meaning, the ability to experience meaning was a basic motivating force of human behavior. We were not taught this stuff at medical school!”
Breitbart became convinced that if he could help patients build meaning, he could decrease their suicidal thoughts and make their lives worth living even to the very end.
He developed an eight-session group therapy program where six to eight cancer patients come together in a counseling workshop. Each session, in one way or another, helps build meaning. In the first session, for example, the patients are asked to reflect on “one or two experiences or moments when life has felt particularly meaningful to you.” In the second session, patients respond to the question “Who am I?” to tap into the identities that give them the most meaning. One woman responded saying, “I’m somebody who can be very private … [and] have been working on accepting love and affection and other gifts from other people.” In subsequent sessions, they share their life story with the group and think about the role that love, beauty, and humor played in their lives.
In the final session, the patients reflect on the part of them that will go on living even after they are dead—their legacy. That could be their soul, or it could be something they helped to create that will continue to exist—their children, a work of art, or an organization. They present a “legacy project” to the group, generally something they do or create that represents how they want to be remembered. One man brought in a woodcut of a heart sculpted into a Celtic Trinity. “This is what I will teach my children,” he said, “that there is eternal love, and that I will be there for them, far beyond my passing.”
Breitbart performed three randomized, controlled experiments on the meaning-centered psychotherapy. When he analyzed the results with his colleagues, Breitbart saw the therapy had been transformative. By the end of the eight sessions, the patients’ attitudes toward life and death had changed. They were less hopeless and anxious about the prospect of death than they were before they began the program. They no longer wanted to die. Their spiritual wellbeing improved. They reported a higher quality of life. And, of course, they found life to be more meaningful. These effects not only persisted over time—they actually got stronger. When Breitbart followed up with one group of patients two months later, he found that their reports of meaning and spiritual wellbeing had increased, while their feelings of anxiety, hopelessness, and desire for death had decreased.
The time between diagnosis and death, Breitbart has found, presents an opportunity for “extraordinary growth.” One woman, for example, was initially devastated by her diagnosis of colon cancer—but after enrolling in the therapy program, she realized, “I didn’t have to work so hard to find the meaning of life. It was being handed to me everywhere I looked.” And that realization ultimately brought her—and Breitbart’s other patients—some measure of peace and consolation as they faced life’s final challenge.
Complete Article HERE!