Here’s Everything You Need to Know

by Sydni Ellis
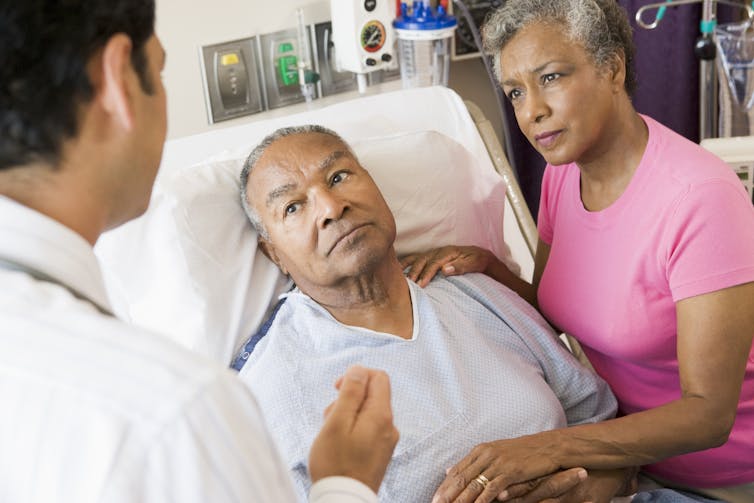
Doulas are compassionate people who help others navigate some of life’s biggest transitions. Some doulas provide support and care to women bringing babies into the world, while others help ease individuals through the difficult and emotional passing of a loved one. These people are known as death doulas, or end-of-life doulas.
Recently, Riley Keough — granddaughter of Elvis and Priscilla Presley — announced on Instagram that she recently completed The Art of Death Midwifery training by Sacred Crossings and is on her way to becoming a certified death doula. In the post, she said, “I think it’s so important to be educated on conscious dying and death the way we educate ourselves on birth and conscious birthing. We prepare ourselves so rigorously for the entrance and have no preparation for our exit.” Riley’s decision to become a death doula comes almost a year after her brother, Benjamin, died by suicide in July 2020 at the age of 27.
Many other women have decided to take on this noble role of helping people in their final days. There are various courses that will certify you as a death doula, including the International End of Life Doula Association (INELDA). This association trains doulas to a high standard of professionalism, where they learn how to listen deeply, work with difficult and complex emotions, explore meaning and legacy, utilize guided imagery and rituals, assist with basic physical care, explain signs and symptoms of last days, guide families through the early days of grieving, and more. We talked to a few death doulas to find out more about this unique profession.
Dana Humphrey, a New York-based life coach and death doula who is certified through INELDA, told POPSUGAR, “Death doulas help the active dying transition with ease. We help them have difficult conversations with their loved ones, so they may say goodbye with grace. We help them figure out their legacy project and help them complete it. We add presence to the dying during a busy hospice environment. We also provide support to the family if they are having a hard time with the transition.”
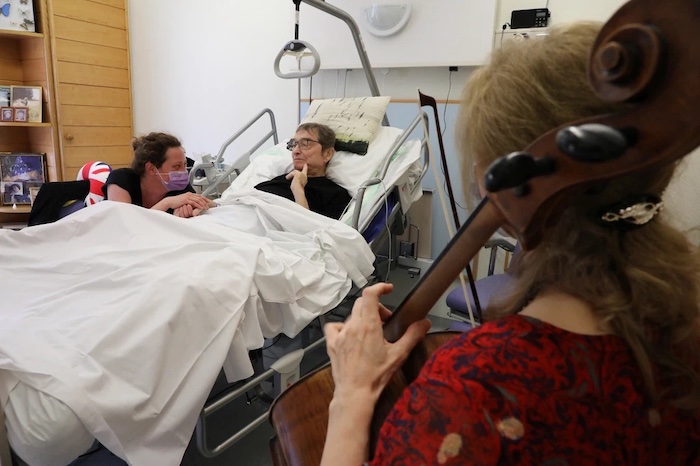
Death doulas are the people that hold the hand of a dying person, ask them about their wishes and try to make them happen, and advocate for them every single day, according to Humphrey. Some of the things she might do include asking the dying person what mood they would like to see and feel when the family comes to visit and then setting that tone, like by having guests take a minute to sit down and move to a place of gratitude before visiting their loved one. Or she might have visitors meet in a “fun station” to put on funny hats or bedazzle themselves in glitter to add lightness in the room.
How Is This Different From Hospice Care?
Suzanne O’Brien, RN, is the founder of the International Doulagivers Institute, who’s mission is to provide awareness, education, support, and programs to communities, patients, and their loved ones worldwide to ensure the most positive elder years and end-of-life process. She told POPSUGAR that a death doula is “a nonmedical person trained to care for someone holistically (physically, emotionally, and spiritually) at the end of life.” This job “recognizes death as a natural, accepted, and honored part of life.”
After years of working as a hospice and oncology nurse, O’Brien felt unfulfilled working hospice, where nurses manage the dying patient’s care but teaches the family how to do the actual 24/7 care. She said she typically didn’t have enough time with patients on hospice as she was only allowed about one hour, once a week with the patient, and she encountered many families afraid of death. This helped her realize that death is “a holistic human experience and not a medical one,” and she wanted to become a death doula instead.
“Every day brings different needs, but it will always center around support,” O’Brien explained. “I will get called by a family whose loved one was just given a terminal diagnosis and they do not know what to do next, or a family whose loved one is actively transitioning and needs more help in the home. [I also get] many calls from families and community members looking for education and resources to help facilitate the most peaceful passing possible.”
How Do Death Doulas Help Marginalized Communities?
Donna Janda, Thanadoula practitioner (another term for death doula) and registered social worker, and Ananda Xela, Thanadoula practitioner and life coach with over 20 years’ experience in social work who has trained with INELDA, both founded Embracing Daisies to empower clients to “see the cycle of life and death not as something to simply rise above but as something to move through with soul and awareness, creating a living and lasting legacy.” They chose this profession to deal with their own feelings about death, as it helped them let death inform the fullness of their own existence, as well as to become part of this burgeoning field in which they didn’t see themselves or other BIPOC well-represented.
“There can be different ways of seeing and dealing with death, and when we talked to both clients within our Black communities and other doulas outside of our communities, we noticed the differences in approach and practice,” Janda and Xela told POPSUGAR. “A lot of the work that takes place in our own communities involves more emphasis on creating comfort around the idea of just talking about death in an honest and open manner before reaching the point of being able to plan for it. It can be a challenge for people who are already in vulnerable positions, historically and personally, to find the desire to face death and accept the idea that it can create more joyful living and offer more control over one’s own narrative — something that is often denied to marginalized peoples.”
Janda and Xela said, “To us, a death doula is someone who can hold space and offer support to both an individual and their loved ones in various areas all along the path between living and dying — from the parts where death seems unimaginable to the parts where it seems inevitable.”
As Thanadoula practitioners, these women hope to aid their clients in seeing that “life and death are connected and give meaning to each other.” They believe that deaths can matter as much as lives, and their job as death doulas is to help patients “discover, create, articulate, and manifest your heart’s wishes.” They also give families space to grieve by taking care of some of the more practical aspects that come from someone nearing the end of life.
What Else Does Someone Need to Know Before Becoming a Death Doula?
If you are thinking about becoming a death doula, you should have a passion for other people, an open-mindedness about death, and the courage to help people through difficult times. O’Brien said, “People often ask, ‘How can you do that work? It must be so depressing.’ I have to say that it is the exact opposite. Working as a death doula has been the hardest thing I have ever done, but the most fulfilling and rewarding. It is an honor and privilege to work with families at this sacred time. What you learn from those at the end of life is wisdom that teaches us about life. It is the best decision I have ever made.”
Complete Article ↪HERE↩!