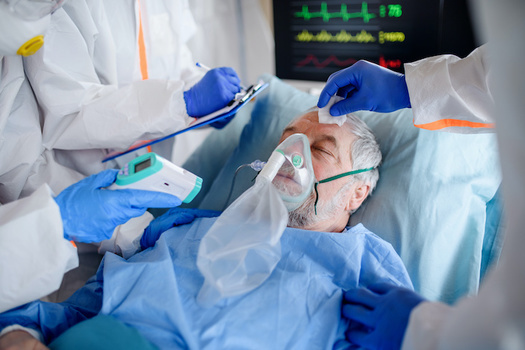
— Without Death, There Is No Life

In the early days of the pandemic, my days were bookended by stories of death. I woke up each day hours before dawn to work on my book manuscript, happy to have a passion project to soothe my anxious energy. My book chronicles how Vermont patients, caregivers and health care providers navigated medical aid-in-dying, in the aftermath of legalization. In the morning, I combed through my notes, writing feverishly about dying, and in the evening, I absorbed the news of bodies accumulating around the world more quickly than they could be buried.
I have never been more acutely aware of my own mortality. I offered my husband detailed instructions about how to tend to my unfinished manuscript, should the need arise. We joked, with gallows humor, about how my death would make an ironic capstone to the book; he, of course, agreed to pen the afterword for the posthumous publication.
Studying medical aid-in-dying, and now living through the greatest pandemic in 100 years, has forced me to reckon with mortality. Over the five years that I’ve collected stories about death and dying, people have often questioned how I could study such a morbid topic. Isn’t it depressing? The answer is, anything but. Humbling and grounding, yes, and at times terribly sad, but never depressing.
An avid reader since childhood, I have always taken great comfort in stories. When the pandemic began, I realized that immersing myself in stories about death had actually helped me. Thinking about my own inevitable death is sad, but it doesn’t terrify me anymore. At 40, I hope I have a great many years left, but I’m also more or less at peace with my finitude.
Yet last spring, when I picked up Natalie Babbitt’s novel “Tuck Everlasting” to read to my 7-year-old son, I realized it was this book that first made me address my mortality, some 30 years ago.
If the concept of mortality was terrifying to me, the idea of immortality was even more so.
Published in 1975, “Tuck Everlasting” takes place in the 19th century, 87 years after the Tuck family unwittingly drinks from a magical spring that renders them immortal. The story is set in motion when a 10-year-old girl, Winnie Foster, accidentally discovers their secret. They bring her to their woodland cottage to persuade her to keep quiet, warning her of the catastrophe that would ensue if news of the spring were to become public.
The novel quickly charmed educators and parents, winning numerous literary awards. While it captivates young readers with its lyrical prose, its matter-of-fact philosophizing on life and death set it apart. In a key scene, Angus, the patriarch of the Tuck family, explains to Winnie that dying is an unavoidable part of the “wheel of life.” The bitter comes with the sweet. It is the difference between having a life and merely being alive. You can’t have living without dying.
The Tucks haunted my childhood. To my 10-year-old self, it seemed clear that the only thing scarier than dying was not dying. How awful it would be to outlive nearly everyone that you love! How bleak it would feel to be resigned to a life of complete social isolation. If the concept of mortality was terrifying to me, the idea of immortality was even more so.
This is precisely what the author had in mind. Babbitt wrote the book to tame the worries of her daughter Lucy, who was then 4-years-old. Babbitt wanted to help Lucy understand that dying was a natural part of the wheel of life, that not dying is much less desirable than it may seem.
Flipping cultural scripts on fears about death: this is the power of stories.
As a non-fiction author, I write for reasons not so different from Babbitt’s. I use real people’s stories to examine cultural fears about death — in my case, about lack of control over dying. Medical aid-in-dying offers what is, for many, a seductive vision of personal control over dying, and the promise of a peaceful, sanitized death. Yet such control often proves illusory, both because access to assisted death is much more complicated than it may seem, and because death, itself, is wily.
People have often questioned how I could study such a morbid topic. Isn’t it depressing? The answer is, anything but.
I think about a woman in her mid-60s I’ll call Candace, who developed metastatic cancer. Once it was clear that she was not going to get better, Candace decided to die on her own terms, with medical assistance. She procured the lethal prescription, which was no easy feat, because many physicians are reluctant to participate in the process. By the time she was ready to die, however, she was no longer able to ingest the medication.
The pandemic has made me even more sure that, like Candace, we are not in control of our destinies. But the Tucks weren’t in control, either. They waited passively, resigned to let the oppressive unfurling of time wash over them. In this sense, immortality’s promise of control over death is also illusory. It is poignant that the Tucks look forward to the day, every 10 years, when their sons return to the family cottage. During the pandemic’s eternal spring, when days bled into weeks and then months, I identified with this feeling, marking my days with UPS deliveries, as time moved ever so slowly.
During the pandemic, I have been in the fortunate position of being able to forestall illness and death with the appropriate precautions, such as staying at home. These measures should permit me to avoid the wrong sort of death. (There is universal agreement at this point that dying from COVID-19 is the wrong sort of death.) But I cannot avoid death altogether, nor (I think) would I want to
Now, 10 months into this crisis, my book is complete. The wheel spins on. The end of the pandemic no longer feels as far off and impossible as it did last spring. And still, I wonder what kind of story I am in. I marvel at that wonder.
Complete Article ↪HERE↩!