
Poor communication, discrimination and lack of training
– Why LGBT people may face inequalities in palliative care
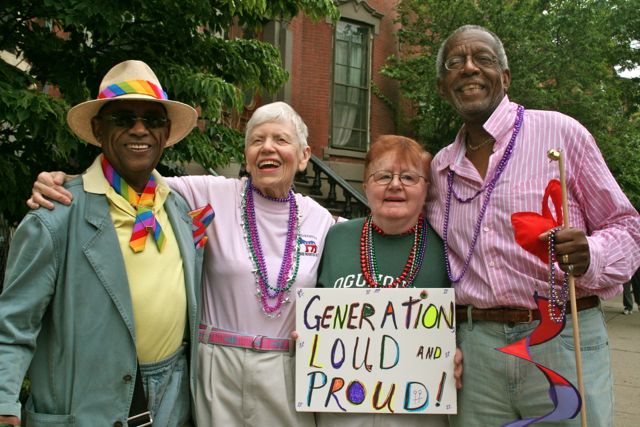
Palliative, or end of life care can help people with terminal conditions, such as cancer, live as well as possible for as long as possible – and allow them to die with dignity. But end of life care is not a straightforward process. And for patients from the LGBT community, the process presents a whole host of barriers that they and their families may face.
Not only do many people from the LGBT community face difficulties accessing high-quality end-of-life care, they also may face issues with their care. This may sometimes be because of ignorance and prejudice against them during pre-hospital admission. It may also be due to poor communication between patients and care providers about treatment plans, judgement by staff about a patient’s family or relationships, and a failure to properly support the spiritual needs of the patient.
Many have also experienced victimisation, discrimination and personal hardship as a result of their sexual identity throughout their life, and may feel that telling a healthcare professional about their sexual identity would change their interactions or quality of treatment.
Staff may also be unaware of an LGBT patient’s particular needs or how to meet them. For example, patients who have undergone gender reassignment may have been married previously in their former gender. They might have children and grandchildren. Dealing with current partners, spouses, former spouses and children during end of life care takes particular skills, which requires specialist training. As many in palliative care want to be surrounded by loved ones, healthcare workers need to be trained to deal with these types of situations.
Many LGBT people may also hide their relationships, meaning that healthcare workers may exclude key individuals from their loved one’s end of life care. Other factors that can impact end of life care include whether an LGBT person lives alone, if they’re socially isolated, and if they face barriers to services or lack consultation. Ageism, and past negative experiences relating to their sexual orientation or gender identity, might also impact the care they receive.
Bereaved LGBT partners and spouses have also been found to experience less support during the death of their loved one. They complained of being shut out of the care process and ignored.
Healthcare professionals also aren’t typically trained to address the specific needs of the LGBT community when it comes to end-of-life care. These needs will include the need for confidentiality and communication from healthcare providers that is sensitive to their sexuality and preferences. Many LGBT people may also feel too vulnerable to disclose their sexual identity while receiving this type of care, which may make their final months lonely.
Room for improvement
Research shows that LGBT people already have lower health outcomes, partly because of ignorance of LGBT issues among healthcare practitioners. For example, they may not receive routine cancer screenings, and may not be able to access adequate healthcare services.
Sexual orientation and gender identity are also both key areas where inequality and discrimination can occur in end of life care. Poor training has been highlighted as one cause.
But many of the shortfalls faced by the LGBT community during palliative care are prohibited and protected by the Human Rights Act 1998. Article three states that no one shall be subject to torture or to inhuman or degrading treatment or punishment, while article eight protects a person’s right to privacy, respect for their sexual identity and the right to control information about their private life.
The issues addressed in articles three and eight have been interpreted by the courts as including how a person plans their end of life care. This means there could potentially be legal redress for any person who feels that their wishes and feelings relating to end of life care aren’t being taken into account by the healthcare workers looking after them.
There are two particular aspects of good end of life care that many LGBT people find are most important to them. First, they want their care to focus on their individual needs. Second, they want their partner to be accepted.
Currently, there are recommendations in place for caring for those from the LGBT community in palliative care. In order to ensure that LGBT people receive the best end of life care going forward, it will be important for healthcare workers to have better training.
Better training will ensure they can communicate properly with LGBT people about their needs and understand their situation. Training will need to include understanding equality, diversity and confidentiality, as well as understanding the unique issues LGBT people face and how this impacts end of life care. Staff or other residents should also report any discrimination to prevent it from continuing in the future.
Complete Article ↪HERE↩!
Anticipatory Grief
-The Fearful Worry About the Future

Today, Mary and I volunteered at the St. Vincent de Paul Food Pantry. I looked forward to getting out of the house and doing more than take a walk. Mary sewed face masks for us and we got gloves to wear when we arrived. Four National Guardsmen were helping. I felt good that I could pitch in and help. Looking at my coworkers wearing face masks and gloves felt a little surreal. I felt grateful for the service of the four Guardsmen wearing protective gear and doing the most dangerous task of loading food boxes into cars.
I can’t believe I just wrote that. Who would have thought loading a car with a box of food is dangerous, even life-threatening? As someone wrote, it feels like we’ve all entered a Stephen King novel. Is this the future? Face Masks? Social Distancing? Gloves? Troops loading cars with food?
What is Anticipatory Grief?
The term for this is “anticipatory grief.” Sam Dylan, in a Healthline article, How Anticipatory Grief May Show Up During the COVID-19 Outbreak, gives us an excellent overview of what this looks and feels like.
1. We feel on edge and are not sure why — hypervigilance; we scan the news regularly.
2. We feel angry and out of control — working at home is not fun anymore, and our favorite brand of mac and cheese hasn’t been available for weeks.
3. We focus on the worst-case scenario — ruminating about an apocalyptic version of the future.
4. We feel exhausted — our worry and stress hormone, cortisol, floods our body and zaps our energy. We read posts about how productive and creative everyone else is, and we find it hard to do anything more than read a novel.
5. We avoid telling anyone how we are feeling. “I am having an awful day today.”
No wonder we have these feelings. We are experiencing a lot of loss. Dr. Doreen Dodgen-Magee identifies loss we experience in her article: Necessary Self Care During COVID: Working through Loss. We’ve lost some financial security, the ability to buy what we want, the opportunity to travel and meet with people. And we’ve lost the feeling that we are in total control of our lives.
Some Things We Can Do.
i. Connect with someone even if we don’t feel like it. Social distancing does not mean cutting off communications.
ii. Name what we are feeling and tell someone about it. “I’m not doing so well today.”
iii. Stay fed, hydrated, rested, and get exercise. Make this a priority.
iv. Try doing something a little creative. Write a poem. Draw a flower. Take some pictures. Start a scrapbook. Learn to knit. Check out YouTube for countless creative ideas.
Step Back a Moment in Compassion.
This is a tough time, and our reactions and the reactions of our family, friends, and neighbors will be different and changing. Instead of lashing out in judgment, try stepping back in compassion. We have some challenging weeks ahead, maybe longer. Instead of looking to a time when it will be over, focus on what is happening right now.
So much is out of our control. Let’s look for what we can control in the here and now.
Complete Article ↪HERE↩!
I Accept Death.
I Hope Doctors and Nurses Will, Too.

A lesson from hospice care might help.
By Theresa Brown
Nurses crying. That’s what I hear from the front lines treating Covid-19 patients. A nurse will begin the shift crying and end it crying. Crying. And we are not a profession that cries easily.
“Untenable” is how the sister of Dr. Lorna Breen, a physician in New York who died by suicide in late April, described her sister’s work situation. She was right. In hospitals with Covid-19 patients, understaffed clinicians often lack sufficient personal protective equipment and tests for the virus, and they fear for their own lives. These conditions would wear on anyone. But they amount to a staggering burden for doctors, nurses and health workers of all kinds whose deeply ingrained duty is to save the lives of their patients.
These medical workers remain devoted to curing and easing the pain of the desperately ill. But what can be done about their pain? Their feelings of failure? Frontline clinicians all over the country are experiencing anxiety, insomnia, a sense of acute inadequacy, and feelings of being betrayed by hospital administrators. Many will likely end up with PTSD. Helplessly watching so many people die, especially when many of them die without their loved ones present, is professionally “untenable.”
We know there is no universally effective treatment for the sickest Covid-19 patients. But their deaths are clearly not the fault of their caregivers. Is it possible to ease clinicians’ burdens so that they feel less personally responsible when these patients die? I believe that another type of care situation, that of a hospice, may offer some lessons.
The most fragile Covid-19 patients are not unlike hospice patients: There is no cure for their condition. While they differ from hospice patients — their deaths often come on suddenly and cannot be foreseen — clinicians might more easily make peace with their deaths by viewing them through a hospice lens.
Even though we are all going to die, death fits uneasily into the world of health care. Fundamentally, health and healing apply to the living, not the dying or the dead, and helping the living get better is why most nurses and doctors got into this work. When I worked in oncology, I saw this principle acted out by physicians who viewed death as failure, and nurses who equated talking honestly about bad prognoses with destroying patients’ hope.
Hospice care approaches death very differently. Practicing as a nurse in home hospice, I understood that patients were going to die. The goal was for them to have the best life possible for as long as possible and to die with minimal distress. Some people associate hospice with “giving up” on dying patients, but that is mistaken. Hospice staff do not hurry death along. Rather, hospice clinicians concede that curative treatment either does not exist for, or has been declined by, the patient, and accept that patients will die under hospice care.
As a hospice nurse, I managed symptoms — pain, trouble breathing, delirium — treated wounds, listened to stories from the past and acknowledged hopes and fears for the future. My intention was that all of my patients would leave this earth without suffering, and though that wasn’t always possible, I tried.
People often say that hospice nurses are angels. I tended to demur and say, “Nope, I’m human.” What the praise shows, I think, is that being comfortable with death is unusual. “Comfortable” is the wrong word: I accept death. I accept its inevitability, but also its importance. Death is the end of each person’s time on earth; it is a privilege to care for people in that moment. I embrace the cycle of life while recognizing the sadness of every death.
(That acceptance is somewhat conditional, though. Two and a half years ago, when I was diagnosed with breast cancer, I chose to take a leave from hospice work. My diagnosis brought the cycle of life a little too close.)
What’s more, a century ago, all of us would have been much more familiar with death than we are now. There were no high-tech emergency departments or I.C.U.s; most people died at home. Modernity made it possible to hide death in hospitals, behind beeping machines and snaking tubes and wires. But now that the entire world is threatened by a previously unknown virus, death has once again come closer.
I am not suggesting that health care workers become indifferent to Covid-19 deaths, or that a certain amount of death from this disease should be callously dismissed as inevitable. No. Instead, I’m urging nurses and doctors to feel less overtly responsible when Covid-19 patients die. As a hospice nurse, I never experienced a patient’s death as failure. Some deaths seemed unjust in a universal sense, like a young mother succumbing to cancer or a dying patient saying she was denied the full scope of cancer treatments because she was black. But the trajectory toward death — I accepted it.
When a patient dies on home hospice, a hospice nurse legally pronounces the death by calling the medical examiner and getting the body released. At pronouncements I did the required paperwork, and I also helped hold, or emotionally contain, the death for everyone gathered. I witnessed the ending of a cherished life and honored loved ones’ grief.
Hospital staff caring for Covid-19 patients need someone to help them hold all the deaths. It is too much to feel responsible for so many imperiled lives, day after day, to rub up against one of the most challenging and often unacknowledged paradoxes of modern health care: Even though we work very hard to heal people, sometimes they still die.
It might be possible to plant a hospice nurse in every Covid-19 I.C.U., but frontline clinicians can also do the work of acceptance by admitting that despite their training, intelligence, tenacity and technology, patients will continue to die of Covid-19. That fact is tragic, and knowing that the mortality rate has been compounded by the failings of our health care system doesn’t help. But it is still possible that the sum of human suffering in this situation can be lessened if nurses and doctors put the blame for their patients’ deaths where they belong — on the virus, not on themselves.
Complete Article ↪HERE↩!
No time like the present
– End-of-life plans and the pandemic

By Sarah Skidmore Sell
Coronavirus has more people addressing their end-of-life planning. And for those who haven’t, it’s a great time to take it on.
People are traditionally rather hesitant to take the steps that experts suggest — creating an advance directive, writing a will and more — in part because they don’t want to ponder their own mortality. But the coronavirus pandemic has sharpened awareness and focused concern on this front. Several estate attorneys, online legal service providers and life insurers say they’ve seen an uptick in interest since the coronavirus hit.
Consider the advice of Jenni Neahring, a kidney specialist and palliative care doctor at St. Charles Hospital in Bend, Oregon who works daily with patients with chronic and serious illnesses. She says it’s better to make these decisions before an emergency to avoid putting extra stress and urgency on loved ones if something should happen.
If a patient is unconscious, health care professionals must spend critical time hunting down relatives or friends to help determine their preferred next steps.
Things have gotten harder with COVID-19, Neahring said, as no one is allowed in the hospitals with these patients and those on ventilators cannot speak for themselves.
“It has brought into sharp relief how necessary these conversations are and how much worse it is to have to do them at the end,” she said.
Here are a few things you can do now to help you and your loved ones later:
POINT PEOPLE
Start with picking your point people: who will make medical decisions for you if you cannot speak for yourself? This person is known as the health care proxy. They will be named in a legal document known as the durable power of attorney for health care.
Then choose someone who can oversee your financial affairs, such as paying your mortgage or other bills, if you are incapacitated. This person would be given financial power of attorney. It doesn’t have to be the same person as your health care proxy.
Choose someone you know well and trust for these roles. Pick a backup as well, in case your first choice is unavailable.
WRITE IT DOWN
After you’ve addressed the health care and financial representatives, consider writing a living will, or “advanced directive.” An advanced directive says exactly what medical care you do and do not want. Each state has its own advanced directive form; they can be found at the Medicare website.
If you are having trouble getting started, check out online resources such as The Conversation Project, Prepare for your Care or AARP’s website.
Consider writing a will to let people know what to do with your assets after you die and who you choose to be guardian of any children. Without a will, it won’t be up to you who raises your kids and your estate could end up in probate, potentially causing more headaches and costs for those you leave behind.
“The takeaway is while this is a current need, it’s always a need,” said Chas Rampenthal, general counsel at LegalZoom.
Many people look at end of life planning, including wills, estates and trusts, as an issue for the wealthy, but that’s untrue, Rampenthal said.
“It’s not about how much you have, it’s about making your wishes known,” he said.
And while life insurance isn’t always considered part of end of life planning, it can be an important step to protect your family financially. Term life insurance, a policy in place for a certain period of time, works best for most families, versus whole life, which is much more expensive and complex.
“This is just prompting people to eat their vitamins and do something they should be doing anyway,” said Peter Colis, cofounder and CEO of Ethos, an online life insurance company.
GETTING HELP
It’s not a great time to meet with people in person. But estate attorney Matthew D’Emilio said that most lawyers are able to arrange phone, video or other consultations during the pandemic. Many states have provided alternatives for witnessing and signing documents to cope with the social distancing rules.
If the idea or cost of seeing an attorney is too daunting, there are many online options for legal documents, some of which provide direct consultation.
SHARE YOUR WISHES
Let your friends and family know what you want, who is in charge and what documents you have. Provide a copy of critical paperwork to your loved ones. Share an advanced directive with your physician as well.
Neahring suggests keeping the name and number of your medical decision maker in your wallet for emergencies.
And while most details will be addressed in the legal documents, some experts suggest writing a short letter reiterating your preferences and reasoning to help provide clarity and comfort to your loved ones later on.
Complete Article ↪HERE↩!
Navigating ‘anticipatory grief’
– how to deal with your lost year

David Kessler, the man who together with Elisabeth Kübler-Ross invented the five stages of grief, says that’s precisely the emotion we’re all struggling with right now. In a powerful interview published on the Harvard Business Review website, Kessler went on to suggest the air was filled with an unprecedented amount of a particular type of grief.
“Anticipatory grief is the feeling we get about what the future holds when we’re uncertain,” he said.
“Anxiety” had never seemed like quite the right word for this moment. It didn’t explain why I could barely look at photos taken just a few months ago, because they made me cry about how we used to frolic on the beach and go out to restaurants and hug people. Nor did it totally summarise the feeling of loss when, on a routine visit to the hospital, I saw nothing along the way but shuttered shopfronts and empty streets.
“I don’t know you, but I miss you” was how I heard it put, which seemed to describe perfectly my longing for the collective undertaking we call society.
How do we get through this without surrendering to the darkness of the moment? Kessler said it was important to bring our thoughts back to the present wherever possible. To simply name five items in the room we’re in, to breathe, and to realise we’re okay right now.
He also said to let go of things we can’t control. Like whether or not we feel a neighbour is practising adequate social distancing, or whether – hypothetically speaking – a president is taking this once-in-a-century crisis seriously enough.
I have been noticing the restorative power of sunlight; the calming quality of a solitary walk; and the absolutely vital service performed in supermarkets.
Things which don’t seem to work as well include texting, because it’s too emotionally ambiguous for big conversations; getting angry at that hypothetical president; and eating too much pizza. There are instead more productive coping mechanisms. Parents who are heroically attempting to home-school their children tell me a schedule is vital. Those of us in book groups are enjoying taking them online. And one Chinese man, Pan Shancu from Hangzhou, ran 50 kilometres in his living room during lockdown by completing 6250 laps around two tables. So what’s your excuse?
Kessler’s last point really stayed with me. He said he has added a sixth stage to the steps in the grieving process, which is Meaning, because “I do believe we find light in these times.” (He also added the often-forgotten caveat that we don’t necessarily move through the stages of grief in a linear fashion.)
A friend put it this way: “People are being forced to see what’s really important in their lives.”
I have been noticing the restorative power of sunlight; the calming quality of a solitary walk; and the absolutely vital service performed in supermarkets and by many other workers keeping the lights on, the water flowing, the internet up. (Never thought I’d be giving thanks for internet service providers, but this is a brave new world.)
Right now there are so many people grieving for the year they thought they were going to have. Maybe you were graduating from university, or getting married, or starting a business, or travelling abroad on a much-anticipated holiday. Or maybe you’re an Olympic athlete who’s spent every waking moment for the past four years preparing for Tokyo. No matter your story, for all of us, it feels entirely appropriate to talk about this virus in terms of what we have lost and will lose. It’s time to give our grief a name.
Complete Article ↪HERE↩!
How to design hospitals for dead and dying people
COVID-19 patients are dying alone. Is there any way to make their experience—and that of their loved ones—less horrifying?

By Erin Peavey and Sheila Ruder
The number of Covid-19 related deaths is rising, a fact accompanied by an equally horrifying truth—many of those who die will do so alone.
Visitors are typically restricted, which means that family members of some coronavirus patients are prohibited from being with them in their last days, unable to touch or hold their loved ones. This scenario is only expected to get worse. According to the Institute for Health Metrics at the University of Washington, as many as 82,000 people in the United States could die from the contagion, while other models show up to 125,000 people. Many health facilities—from traditional hospitals to makeshift alternative care sites—will have to decide how best to provide dignified end-of-life care to COVID-19 patients and their loved ones.
The two of us have collectively worked in healthcare architecture and research for more than 30 years and have worked nationally and internationally on palliative care solutions in a variety of healthcare settings. We also both recently lost loved ones. We know firsthand how important compassionate end-of-life care is. Yet existing guidelines from Centers for Disease Control on alternative care sites—the very places many acute COVID-19 patients are dying—do little to address it. Here’s how traditional and nontraditional care spaces alike can create safe, comfortable end-of-life experiences, even when resources are stretched thin.
A comfortable environment
Support privacy
Having a degree of privacy is crucial so that each patient can say goodbye to loved ones or have religious rites. This can be done in-person or, more likely these days, virtually. (Some facilities do allow a visitor for end-of-life cases, with the provision that visitors wear personal protective equipment.) Normally, patients get a private room, but many hospitals are overrun and simply don’t have the space. Instead, hospitals and makeshift medical facilities could provide a simple curtain or a divider between beds.
Family visits
Establishing protocols for visits is important, so patients and family alike know what to expect. Facilities should clearly communicate whether visitors are allowed in person or virtually, what visiting hours are, how many visitors are allowed, and what sort of screening they need to pass. There should also be clear direction around mementos or spiritual items that family may want to pass to their loved one: Are they allowed or not? How should they be handled?
Support two-way communication
If family members are not allowed to visit physically, care centers can support other ways loved ones can say last goodbyes, such as two-way video communication, or visual contact through a protective barrier, like a window.
Positive distraction
Personalized acoustics or comforting nature sounds can go a long way toward making a patient feel comfortable. Many of the makeshift hospitals that have been built to support COVID-19 patients are bare bones and don’t support elaborate sound systems. But headphones or bed speakers can work just as well. When patients are conscious, access to sunlight, nature, or images of nature can also be soothing.
Hospice caregivers
Dedicated hospice workers can manage the caring aspect of end-of-life care when resources across the system are under siege. Staff qualified to tend to very sick patients should remain in those designated areas.
How to create a safe environment
Building dignity into end-of-life care is only part of the solution. Care facilities also have an imperative to prevent spreading the virus further. Here are some key considerations.
Medication access
Narcotic drugs should be securely stored but located so caregivers can reach them easily. The medication may be placed in a locked cabinet at a designated staff workstation near patient care areas, for instance.
Dedicated entry
For facilities that allow family members to say their final goodbyes in person, providing a dedicated entry to the space can reduce the chance of transmission. Mobile handwashing stations can also be provided throughout the facility. Donning and doffing zones should be established for any staff and family members entering or exiting the facility.
Staff accommodations
Dedicated toilet rooms and respite areas can be provided for healthcare workers. The death of a patient can be difficult for even the most experienced caregivers and they, too, need space to process their pain.
Back-of-house access
When patients die, they should be removed discreetly from the facility, through a separate exit. This is not only to preserve their dignity and avoid frightening visitors and other patients. It’s the safest approach to prevent spreading the coronavirus.
None of these are new ideas in healthcare design, but as hospitals rush to treat legions of new COVID 19 patients, they have to embrace the reality that many patients will succumb to the virus and their families will suffer. There are ways to help ease that suffering in a compassionate way.
Complete Article ↪HERE↩!
